

Canadian
maple
Medical Alliance for the Preservation of the Lower Extremity

Neuropathic / Diabetic Ulceration Treatment
Neuropathic ulcerations (also known as neurotrophic ulcers) are caused by
neuropathy, an abnormal functioning in the nerves of the feet.
There are several nerve pathways that can be affected by neuropathy, but the
most important is a loss of sensation in the feet. When this is severe enough,
the patient may not feel excessive pressure and friction, something we call
'loss of protective sensation," or LOPS.
These are the patients who are susceptible to neuropathic wounds.
Diabetes is the most common cause of neuropathic ulcers. In fact, diabetes is
a more common cause of neuropathy and neuropathic wounds than all other
causes combined. So common is diabetes as a cause of neuropathic wounds
that there is an almost instant assumption that any neuropathic wound is most
likely caused from diabetes. You can read about the daunting statistics with
diabetes here.
But there are many other causes of neuropathy that may lead to a
neuropathic foot wound.
Patients with a past or current history of alcohol abuse commonly
develop these wounds as well.
In photo 2 to the right, we see an infected neuropathic ulcer at the
tip of the toe caused by past alcohol abuse. Both the ulcer and the
infection extended down to bone, and it was spreading up the leg.
Note the redness on the leg, representing a spreading infection. It
was treated with IV antibiotics and local wound care.
Kidney disease may also cause neuropathy that may lead to wounds
(though many kidney disease patients also have diabetes--over 60%
in the author's Health Authority). Below is an end-stage kidney
disease patient with two ulcers that communicate with each other.
This required surgical intervention to remodel the amputation.
Vitamin deficiencies, rheumatological conditions, spinal
compressions and injuries can also lead to neuropathic
wounds.
And a surprising number of neuropathic wounds are
idiopathic in nature--meaning there is no known cause to
the neuropathy. To the right we see such a patient. He
has a deep wound extending to bone. He is completely
insensate (without sensation), yet there has been no
cause identified for the lack of sensation.
You can read more about the various forms of neuropathy
here.
The lesson is that if you are a diabetic or are at similar risk for
neuropathy, it is important to be screened regularly for the
a loss of sensation that can put you at risk of ulcer formation.
Other Factors Affecting Neuropathy
Besides the sensory loss of neuropathy, there are other factors
in neuropathic ulcer formation as well.
The blood supply to the foot plays a huge role in terms of how
well the body can respond to the physical insult that may cause
an ulcer, and provide the tools for healing. So too, with blood
sugar levels and nutritional status.
From a mechanical perspective, the greater the amount of time
one spends on one's foot is certainly correlated with a greater
likelihood of an ulcer. So a weight-bearing job, particularly on
concrete, heightens risk.
So, too, does body weight.
And there are a host of biomechanical factors (positions and
movements of the foot) are also at play in ulcer formation, which
we discuss here.
How Severe Can The Sensory Loss Of Neuropathy Be?
The degree of sensory loss in neuropathic patients can be quite
profound.
In many cases, we can perform surgery, even amputations, without
the need for anesthesia.
In photo 5, above right, a patient who has already experienced
the amputation of two toes, was surprised to learn he had a new
ulcer and was walking around on exposed bone.
In photo 6, the example to the right, the patient knew there was
an ulcer on his toe, and he knew bone was sticking through the
wound. However, he never bothered to have it treated because
it was painless. He had been walking on this foot for four weeks,
coming in to the hospital for dialysis three times per week for
dialysis, but didn't think to mention it to a doctor.
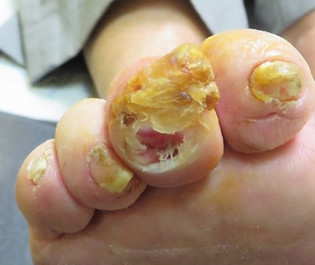
In photo 7, the patient had been treating this toe bone protruding
through the skin as a "callus," but came in for a consultation after
it didn't heal in 6 weeks.
In photo 8, we see a patient whose foot felt cold (a symptom of
neuropathy). He placed his foot on a space heater, and it burned
his skin to the extent it exposed three toe bones on three toes.
Not only did he feel cold because of neuropathy, he couldn't feel
the damage of the space heater because of neuropathy, too.
He felt because there was no pain, it couldn't be that serious. And
because it didn't hurt, he refused to take time of from his work as
an apartment manager, even though the job has weight-bearing
responsibilities. We removed his three toe bones and he healed
without issue, still never taking a day off work.
How Does The Skin Break Down To Create An Ulcer?
This is a big enough topic that we devote a web page to that
topic here.
Where do neuropathic wounds develop?
Neuropathic wounds are caused by a combination of neuropathy and a mechanical force--pressure or friction (shear). So these wounds are almost always found on the weight-bearing surface of the foot. While neuropathic wound can appear anywhere on the foot, between 75 and 80% are found in the toes or ball of the foot.
The single most common location of a neuropathic ulcer is the medial side of the great toe, as seen in photos 9-11 below. We discuss a the reasons this is so on our page on biomechanical causes of neuropathic foot ulcerations.
Alternatively, neuropathic ulcers
may develop at a pressure point
on the tip of the toe (12), or the
top of a toe (13).
The cause of ulcers in the smaller
toes, too, is discussed on our page
on biomechanics and ulcer formation.
The ball of the foot (the metatarsal region) is a common site for ulcers to form, too. They can occur anywhere in this region, but are most common beneath the 1st and 2nd metatarsal heads (the bones to which the 1st and 2nd toes attach to the foot.)
The reason ulcers form where they do comes down to foot function. The 1st metatarsal region is a common site for neuropathic ulcers to form because this is the biggest metatarsal bone, and because the large toe is the primary push off point in gait. Stiffness in the motion of the big toe, and large bony prominences in the toe are a couple other causes for ulcers at this site.
The 2nd metatarsal is a common site of ulcer
formation, too, because this is the longest
metatarsal. And sometimes the 1st metatarsal
is overly mobile and elevates in gait, leaving
the 2nd metatarsal to bear more weight.
It's also common to see ulcers here when
the 2nd toe is contracted, pushing weight
down on this bone.
To the right we see examples of neuropathic
ulcerations at these sites.
The near right photo (14) shows an ulcer at the
level of the 1st metatarsal head (big toe joint).
To the far right, (15) there is an ulcer beneath the
2nd metatarsal head (base of the 2nd toe joint).
You can have neuropathic ulcers at the other
metatarsal heads too. To the near right (16)
is an ulcer beneath the 3rd metatarsal head
(3rd toe joint). The 3rd and 4th metatarsal
heads commonly develop ulcers when the
toes are contracted, thereby putting more
pressure down on to this bone, or if the
metatarsal bone is positioned lower than
the other metatarsal bones.
To the far right (17) we see an ulcer beneath
the 5th metatarsal head (little toe joint). This
location is a common site for neuropathic
ulcers to form when the foot strikes the
ground in an inverted orientation.
The redness and swelling around the ulcer on
the far right suggest infection. Pain would
accompany an infection in most patients, but
it often not present in patients with neuropathy.
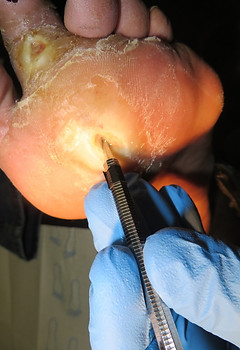
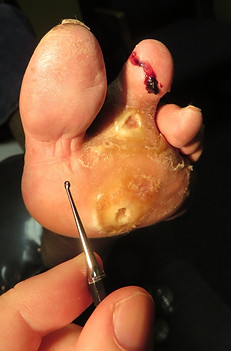
Ulcers in this region can extend quite deep.
In photos 18 and 19, the ulcer could be probed
all the way through the foot, with the probe
tenting up the skin on the top of the foot.
Amputation was recommended at his local
hospital. But the patient refused. It would
mean he couldn't work or support his family.
This wound was healed with offloading with
a total contact cast (TCC), and as of five years
later he is still working on his feet as a contractor.
This shows the importance of having podiatric
wound specialists in the hospital to determine
what feet can be salvaged. Because there are
few true foot specialists in Canadian hospitals,
people give up on healing too soon, and
amputations are suggested much too quickly.
Neuropathic ulcers can also occur in the midfoot and rearfoot. Below left, 20, is a heel ulcer caused by weak calf muscles that increase pressure here. Below center, 21, is a heel ulcer treated for three years with dressing changes. It was closed with offloading and maintained an accommodative orthotic (one that removes pressure from the heel.) Below right, 22, is an ulcer in the midfoot caused by Charcot neuroarthropathy, where the arch of the foot collapses abnormally. Charcot is a very interesting topic that is covered in more detail here.
As you can see, neuropathic ulcers can occur in a variety of areas of the foot. It's
important to understand the biomechanical cause of each neuropathic wound
because if the cause is not addressed, the wounds tend not to heal, or won't stay
healed. Podiatrists are particularly adept at understanding the underlying
biomechanical cause of a wound.
We briefly discuss the topic of the biomechanics of wound formation here.
Calluses and Neuropathic Wounds
If you notice, many of these ulcers have calluses associated with the wound.
Maybe around the edges, maybe over the ulcer itself.
When caused primarily by pressure, neuropathic wounds are commonly circular
in shape. When caused by shear, they may be more elliptical in shape. And
because neuropathic wounds have a mechanical component (pressure and/or
shear), they are typically surrounded by, and sometimes covered by, a layer of
callus (thick skin).
Calluses are not conducive to healing. Because they can cover a wound, it is
often difficult to tell if an ulcer is even present. If the ulcer is present, calluses
may make it hard to assess the depth or extent of the wound.
Calluses also put more pressure on the wound, which is the cause of these
sorts of wounds. And calluses can contribute to shear forces--friction that can
cause tearing of flesh. (You can read more about the mechanical forces that
cause wounds here.)
And calluses are dead tissue, a food source for bacteria, which we aim to
discourage. And if calluses cover an infected wound, they can seal bacteria
inside, allowing any infection present to do more damage.
If you look at photo 23, does this look like a plain thick callus? Or is there an
ulcer beneath? Does it look infected?
Even for experienced physicians, it's often hard to tell.
In this case, there was an ulcer under the wound, and it extended to bone.
The patient had a chronic bone infection (osteomyelitis), yet exhibited little
to suggest an infection.
There would be little way to know what was going on with the foot if the
callus wasn't debrided. In fact, an identical callus on the other foot had no
ulcer.
So calluses must be removed, both to see what's going on with a wound,
and to give the wound the opportunity to heal.
Removal of this dead material is called 'debridement' and is vital to neuropathic wound healing. Unfortunately, it is commonly ignored tenet of wound healing, simply because few doctors or nurses in Canada are trained in how to do it.
Some physicians will debride a wound, though few do it routinely. Some specially-trained nurses will do it, so long as it doesn't extend too deep. Podiatrists, particularly those who specialize in wounds, are particularly adept at debriding ulcers, but unfortunately, most provincial health plans do not insure this service.
But debridement needs to be done on every neuropathic foot with a callus.
So, what do you do when you see a callus?
We tell our patients that the very word "callus" literally tells the patient what to do--"Call us"!
-
Call us before the ulcer develops under the callus.
-
Call us to get an assessment of the extent and status of any ulcer beneath the callus.
-
And call us to remove the callus to give any underlying ulcer the opportunity heal.
Beyond debridement, the other major tenets of neuropathic wound healing are offloading, dressings and infection control.
Please explore those links.
If you'd like to learn how pressure and friction cause the skin to break down and form an ulcer, please visit this page.
Click the maple leaf below to return to the top of the page.
"Turn your wounds into wisdom."
-- Oprah Winfrey















1
2
4
5
6
7
8
16
19
9
10
11
12
13
14
15
17
18
19

20

21

22

23
This page written by Dr. S A Schumacher
Podiatric Surgeon
Surrey, British Columbia Canada
All clinical photographs owned and provided
by Dr. S A Schumacher. They may be reproduced
for educational purposes with attribution to:
Dr. S A Schumacher, Surrey, BC Canada
and a link to this website, www.CanadianMAPLE.org.
