

Canadian
maple
Medical Alliance for the Preservation of the Lower Extremity
Effects of Neuropathy
We defined neuropathy as a pathology within the nerve and discussed some of the many possible causes of neuropathy here. On this page we discuss what effects neuropathy has on our bodies.
What symptoms Occur with Neuropathy?
There are three main types of neuropathy--Sensory Neuropathy, Motor Neuropathy, and Autonomic Neuropathy.
We'll discuss them from the least known (autonomic) to the best known (sensory).
Autonomic Neuropathy
Autonomic nerves control things you don’t think about.
For example, your blood pressure, respiration, and heart
are controlled by autonomic nerves. And an autonomic
neuropathy may result in high blood pressure (hypertension),
dizziness or fainting and difficulty breathing. Autonomic
neuropathy may cause an abnormal or irregular heart rate.


Our eyes' ability to adjust to dim light is controlled by
autonomic nerves, and neuropathic patients may have blurred vision and difficulty focusing their eyes.
They may have difficulty driving in the dark.
Autonomic nerves control how food moves through your
digestive system (Peristalsis) and how food is processed.
So patients with autonomic neuropathy may experience
altered digestion, diarrhea or constipation, nausea,
altered appetite, bloating, difficulty in swallowing, abdominal pain, or difficulty in swallowing.

Urination is controlled by autonomic nerves and autonomic neuropathy may result in incontinence or an inability to empty the bladder.
Sexual function is mediated by autonomic nerves and can be adversely affected by neuropathy.
Perspiration is controlled by autonomic nerves as well, and
abnormalities in perspiration can be an result of neuropathy.
It may be difficult for a person to regulate their body temperature--becoming heat intolerant.
One observable sign of neuropathy is excessive perspiration
with eating, something known as gustatory perspiration. It
is similar in appearance to the sweating seen when someone
is eating spicy food, except in the neuropathic patient, it is
seen when eating any meal.
So keep an eye on the forehead of a diabetic when he is
eating and you may witness this phenomenon.

In the lower extremities, patients with an autonomic neuropathy may exhibit excessive sweating, or extremely
dry skin (below left and right). So if you have an autonomic neuropathy and dry skin, make certain to moisturize
appropriately.


By altering moisture content, neuropathy can thus weaken
the skin, creating small cracks that make it more susceptible
to fungal infection, bacterial infection--and ulceration.
Autonomic nerves also control blood flow, and thus, autonomic neuropathy can affect blood flow to the feet.
The vessels may be open (patent), but the blood may be shunted back to the heart prematurely
In the image to the right, we see the white, blanched skin of the toes, indicating poor blood flow from the nerves clamping down on the flow to the toes.
The toes may feel cold and uncomfortable. Diminished blood flow certainly inhibits the body's ability to repair injury.
In severe cases, as seen below, neuropathy can result in circulation so poor that the tips of the toes may even turn black and die--gangrene.




Motor Neuropathy

Neuropathy may affect the motor nerves—the nerves heading from the brain to the extremities (hands and feet). In the foot, this may result in hammertoes, bunions, or an abnormal arch structure. This may cause increased pressure under bony prominences, that predisposes a patient to ulceration.
To the left we see tight tendons on the top of the foot caused from motor neuropathy. Abnormal nerve signals sent to the muscles cause the toes to contract and twist in odd directions.
As this progresses, ulcers could form on the top of the toe (below left) or on the tip of the toe (below).



To the left we see a contracted large toe. As the toe gets pulled upwards, it puts a retrograde force back
on the ball of the foot. This has created a callus, and
is a potential site of a future ulcer.
This pressure site could be offloaded with an orthotic or a specialized shoe. It could also be surgically corrected to realign the bones and prevent the mechanical forces that might cause the ulcer.
Neuropathic contractures can be quite significant.
Imagine the increase in pressure exerted on the
ball of the foot when the patient to the right stands
up.
Imagine how the toes fit in a regular shoe.
Neuropathic-induced deformities can increase the
chances of ulceration and infection.

Motor neuropathy can also change biomechanics -- the
movement function of the body. An example can be
seen to the right, where the foot pronates, or rolls
inwards too much.
This foot will be exposed to increased pressure and
friction forces, the physical forces creating ulcers.
But abnormal mechanical function of the body like this
may also create issues higher up.


When one foot pronates (rolls in) excessively,
the arch flattens and the leg and thigh rotate
inwards.
This may cause the pelvis, which sits on top of
the thigh bone to roll forward, down, and
become tilted (left).
The vertebrae (the bones of the spine) rest on the pelvis. So a tilted pelvis could, in turn, cause the vertebrae to become misaligned. A previously straight spine (below left) may become crooked and misaligned (below right), a condition known as scoliosis. Such a deformity may compress nerves as they leave the spine, causing further nerve dysfunction.


Patients with motor neuropathy may also move more clumsily and be more prone to falls.
So severe is the motor neuropathy of the patient to the right that he needs both an ankle brace and a walker to get around.

Sensory Neuropathy
Neuropathy may also present as sensory neuropathy—damage to the nerves coming from the extremities towards the brain. And it may present in opposite ways.
Painful Neuropathy
Some patients develop an increase in painful sensations. Hyperalgesia is exaggerated pain sensations to things that are normally uncomfortable. Allodynia is pain from something that should not be painful, like a light touch or the pressure of a bedsheet.
Paresthesia is the abnormal sensation of tingling or "pins and needles” sensations.
This can be irritating to some. In others it can be quite uncomfortable to disabling.
"And I get down on my knees and pray,
that they go away
And still it begins, needles and pins."
--"Needles and Pins"
The Ramones
Sometimes there is just pain. Constant, unrelenting pain, unassociated with any stimulus. No injury. No wound. Just pain.
There are many medications that can be used to treat this pain, both topically (applied to the skin) and through oral medication, though the efficacy varies.
Sensory Loss
More commonly, and most importantly for patients with ulcerations on the foot, sensory neuropathy may experience sensory loss--a lack of sensation, or numbness.
This, too can become profound. Many doctors in the wound care field can relate stories of having found needles, pins, thumbtacks, and nails in the foot without the patient noticing.
“Indifference and neglect often do much more
damage than outright dislike”
-- Albus Dubledore
An inability to feel pain (Loss of Protective Sensation) makes it easy for patients to neglect caring for their feet, to become inattentive to damage their feet may develop.
This patient presented to our hospital three times per week for dialysis. When he was sent to our podiatric service, his toe bone was sticking out of his toe.
He told me it had been like this for 3 months, but it didn't bother him enough to mention to his doctor for referral.


To the right is a neuropathic patient who went for a 5-km walk with tight shoes and no socks.
His wife noticed the damage, not the patient.

Here we see a patient who used a slip-on shoe with a tight toe box and no socks.
She had already lost two toes on her opposite foot but didn't notice this issue on her left foot. She came in for another problem.
This patient, too, presented with a toe bone sticking out of her toe.
She couldn't feel any pain and assumed the lump on the top of the 4th toe was simply a callus.

“Just because you can't see the wound doesn't mean it isn't hurting.”
-- Jodi Picoult, The Pact
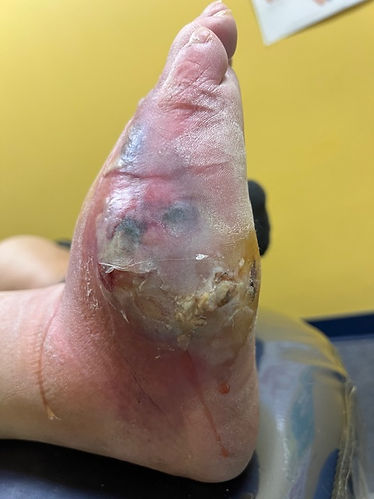
For many neuropathic patients, sensory loss simply means they cannot feel when they've been on their feet too much. They don't feel pain that the rest of us may feel, and can't tell when the skin is becoming bruised, breaking down and an ulcer is developing, as seen below right.
The patient below left was completely unaware of the large ulcer on his right foot. He can't see the dirt, dog hair, and other foreign material contaminating the wound. And he can't feel discomfort.
The patient below right presented with a severe, limb-threatening foot infection. Not only was he unaware there was an ulcer (let alone an infection), he had to be convinced to go to the hospital for IV antibiotics as he had a round of golf scheduled for the following day.

The author of this web page once found a jack (as with the children's game ball and jacks, right) inside a 36-year-old female patient's heelbone.
The patient couldn't feel having stepped on it; she only noticed the problem because of the smell of the infection that developed.

And the author has had more than one patient pull their foot out of their shoes and leave a toe behind, without noticing anything amiss.
In many cases, amputations can be performed in the neuropathic patient, without the need for anesthesia, so profound is the neuropathy.
Insensitivity to Temperature
As pain and temperature run up the same nerves, patients
with neuropathy commonly cannot feel the cold.
Sometimes patients brag about being tough enough that they were able to walk barefoot across the snow to get the mail or take out the trash.
In reality, their feet were simply numb from the loss of nerve
function from neuropathy, and they were causing themselves
harm.


The author of this web page had a patient who had already undergone the amputation of two toes, and was quite distraught when he developed a new ulcer on the bottom of his foot, thinking he might now lose a leg.
It took over two months for us to get the ulcer healed.
The patient was so happy, he rewarded himself by going fishing. He stood in the river in waders, large boots that allow you to wade out into the water without getting your feet wet.
The waders kept the feet dry successfully.
But even in the summer, the rivers of British Columbia run
cold, and the patient couldn't feel the thermal damage on
his toe.
The toe became infected with a resistant organism, and the
patient passed away from the infection that resulted from
this wound.
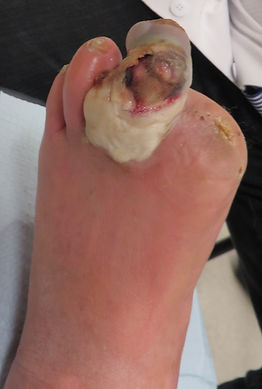
Below we see a patient who, in the middle of summer, felt his feet were excessively cold. He put his feet against a heater. He couldn't feel the damage.
He presented with gangrene of the tips of his middle three toes of his left foot (below left). When the black skin sloughed off (below right), bones were visible in two of the toes. We removed the bones, and the patient recovered without issue. But at no point did the patient take a single day off work. It didn't hurt, so he refused to believe, it was a major issue.


At times the problem is just the opposite. Sometimes neuropathic patients may also feel their feet are cold, when they are not.
Combine this with an inability to feel heat, and a greater fragility of tissues, and you have a problem.
The author of this webpage
once saw a woman who
went into a hot tub with
her husband.
She had neuropathy. He did not.
She came out with enough
skin damage that she
required substantial skin
grafts on her feet and legs.

He emerged from the same hot tub without ill effect.
Effects of Altered Sensation on Walking
Below left we see an x-ray of a normal ankle joint.
The patient pictured below right presented to the author's office complaining of instability in his ankle while walking.
He required a cane to help support him, but he told me he knew it wasn't serious because there was no pain.
Even after the x-rays came back and the patient he was informed he had suffered a devastating, limb-threatening comminuted ankle fracture, he was convinced it was probably just a sprain.


Patients with sensory loss often find walking more difficult, in that they cannot feel the ground, another major component in instability.
To the right is a patient who cannot feel the ground when he walks, and this has given him an abnormal, swaying gait.
He works in construction, and he has such poor sensation that he falls frequently at work, often just from walking.
His co-workers have accused him of being drunk.
It's no longer safe for him to be on a ladder.
It's better for him during the day when he can use his eyes to reorient his position. At night, or when he is in a dark room, he can neither feel the ground nor use his eyes to reorient his body position, and he is particularly vulnerable to falling. With the poorer circulation, poorer healing, and weaker bones of advancing age, the falls will become increasingly dangerous.
Sensory loss is the single biggest factor in the development of ulcers, and without neuropathy, ulcers are very unlikely to develop. But when we combine sensory loss with new bony prominences and abnormal gait from motor neuropathy and dry, less resilient skin from autonomic neuropathy and it's easy to see how foot ulcers develop.
We've devoted a page to neuropathic ulcerations here. And we describe how the skin breaks down with neuropathy here.
Further complicating matters, diabetics often develop diabetic retinopathies (eye damage), too, which may adversely affect their vision.
So not only may they not be able to feel that something is wrong with their feet, they often cannot see the problems either.
And with age, stiffness, arthritis, and weight gain, they may not be able to bend to reach and care for their feet either, even if they see a problem.

In Summary
So motor neuropathy can cause the toes to contract and the gait to become altered.
Autonomic neuropathy can cause the skin to become dry and compromised, susceptible to trauma, ulcerations and infections. It can also diminish blood flow to the feet, particularly the toes, making it difficult for the body to repair this damage.
And sensory neuropathy can dull the sensations that should warn the patient that any of this is happening. This makes the neuropathic patient more likely to ignore these harmful processes, where as with the ability to feel pain, we would listen to the warning signs of this damage.
"Pain we obey"
--Marcel Proust
To return to the top of the page,
click on the maple leaf to the right.
This page written by Dr. S A Schumacher
Podiatric Surgeon
Surrey, British Columbia Canada
Unless otherwise indicated, all clinical
photographs owned and provided by
Dr. S A Schumacher.
They may be reproduced for educational
purposes with attribution to:
Dr. S A Schumacher
