

Canadian
maple
Medical Alliance for the Preservation of the Lower Extremity

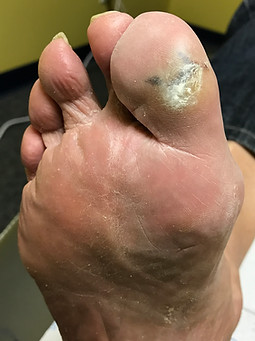
Look at it from your body's perspective. An ulceration like the one to the right, develops on the bottom of the foot from pressure and friction.
The body produces fragile skin cells in the attempt to heal a wound, all the while fighting off bacteria that have entered the wound.
And because neuropathic patients can't feel pain, they don't know there is a problem. So they walk on the foot, with every step applying the weight of our entire body on those fragile skin cells, destroying them with each step.
So how can ulcers be offloaded?
There are many ways to offload, or remove pressure from an ulceration, and each has pluses and minuses. Statistically, the most effective way of getting an ulcer to heal is with a non-removable device, such as a total contact cast or a non-removable walking boot. But these may not be practical in all cases.
So the best choice in an individual case depends upon factors such as the severity of the wound, the location of the wound, the age, health, and fitness of the patient. We'll review a variety of ways wounds are offloaded, discuss the pluses and minuses of each, and give you some recommendations.
Let's start with some common techniques for simpler wounds.
Accommodative Felt Padding
Offloading may be achieved with accommodative padding to redistribute weight from a wound. This is sometimes known as a poor-man's cast.
The way it is done is by placing a thick piece of felt or similar non-compressive material around the wound, (but not on the wound), as seen in the two patients below. On the left is a thick pad offloading a 4th metatarsal head (the bone to which the 4th toe attaches) before a wound bandage and cover is applied. To the right is a pad offloading the 2nd metatarsal head (where the 2nd toe attaches to the foot), with the dressing and cover applied.
Offloading
(Removing Pressure and Friction From An Ulcer)
If there's on thing to learn from this website it is this:
For most neuropathic wounds, the single most important
factor in wound healing is offloading.
If you can remember that, you'll know how to heal most
neuropathic / diabetic wounds.
So what is offloading?
Offloading is the removal of pressure and friction from a wound.
And it is important because neuropathic wounds are caused by a combination of neuropathy (the loss of normal sensation that serves to warn us of damage to our feet), combined with pressure and friction (shear)--the forces that damage our feet.
At this point in time, medicine cannot cure the sensory loss neuropathy. So we must control the other side of that equation--the pressure and shear. And removing pressure and shear from a wound is the definition of offloading.
"It’s not what you put on the wound
(like medications and bandages) that counts. It’s what you take off (like dead tissue and body weight)."
--Paul Brand, MD
Pioneer in Wound Care


The idea is to redistribute weight away from the ulcer by building up the surrounding areas so that area bears more weight. In these examples the felt is 1/4" thick, though different thicknesses may be used.
A dressing of some sort is applied over the wound. Perhaps it's a simple non-adherent bandage, perhaps it's a dressing to add or remove moisture, perhaps the dressing is something else. The felt pad and wound dressing would then be covered over in some fashion, as you see in the photo on the upper right.
Felt padding has fallen out of favor for some, as it takes time from the clinician to apply.
Yet several studies show felt is quite effective. In particular, a 2025 US study, Tong et al found that 78% of ulcers were healed by 12 weeks with a median 45 days to heal.
Tong KP, Obradovic KN, Acciani AL, Wortzman N, Kigner S. The use of multilayer felt padding in the treatment of neuropathic plantar foot ulcerations. J Am Podiatr Med Assoc. 2025 Jan–Feb;115(1):22-088. doi:10.7547/22-088
In a 2002 study out of LSU, researchers found that 81% of forefoot wounds healed within 12 weeks if treated by felt.
Birke JA, Pavich MA, Patout CA Jr, Horswell R. Comparison of forefoot ulcer healing using alternative off-loading methods in patients with diabetes mellitus. Adv Skin Wound Care 2002 Sep-Oct;15(5):210-5.
Other studies show how ifelt diminishes pressure.
Zimny S, Meyer MF, Schatz H, Pfohl M. Applied felted foam for plantar pressure relief is an efficient therapy in neuropathic diabetic foot ulcers. Exp Clin Endocrinol Diabetes. 2002 Oct;110(7):325-8. PubMed PMID: 12397530.
Nube V, Molyneux L, Bolton T, Palmer E, Yue D. The use of deflective padding in the management of plantar hallux and forefoot ulcers in people with diabetes. Foot. 2006;16(1):38–43. doi: 10.1016/j.foot.2005.11.005.
As one might imagine, thicker accommodative felt padding applied around the wound reduces pressure on an ulcer by a greater degree than thinner padding.
Curran, M, Ratcliffe, C; Campbell, J A comparison of types and thicknesses of adhesive felt padding in the reduction of peak plantar pressure of the foot: a case report. J Med Case Rep. 2015; 9: 203. Published online 2015 Sep 24. doi: 10.1186/s13256-015-0675-8 PMCID: PMC4581116 PMID: 26400619
This is one reason that studies suggest that padding reduces pressure by varying amounts. For example, on the lower end, this British study found that peak pressure (PP) and pressure time integral (PTI) at the ulcer site was cut by 25%-29%.
Paton J, Woodrow T, Passmore C. The effect of plantar cover padding with U'd cut-out on plantar foot pressure; preliminary study. Brit J Podiatry. 2007;10(3):110–5
This Australian study found pressures dropped by 49% with accommodative padding.
Raspovic A, Waller K, Wong, WM The effectiveness of felt padding for offloading diabetes-related foot ulcers, at baseline and after one week of wear Diabetes Research and Clinical Practice November 2016 Volume 121, Pages 166-172 DOI: https://doi.org/10.1016/j.diabres.2016.09.018
And this German study found accommodative padding reduced pressure by 70%, from 297.3 ± 120.0 kPa before to 90.3 ± 38.2 kPa.
Zimny S, Reinsch B, Schatz H, Pfohl M. Effects of felted foam on plantar pressures in the treatment of neuropathic diabetic foot ulcers. Diabetes Care. 2001;24(12):2153–4. doi: 10.2337/diacare.24.12.2153.
And as you might expect, because felt tends to compress with time, newly-applied padding diminishes pressure on a wound better than worn padding.
Pressure averaged 367.2 kPa with no padding; 188.0 kPa with fresh padding; 248 kPa with worn padding.
Raspovic A, Waller K, Wong, WM The effectiveness of felt padding for offloading diabetes-related foot ulcers, at baseline and after one week of wear Diabetes Research and Clinical Practice November 2016 Volume 121, Pages 166-172
DOI: https://doi.org/10.1016/j.diabres.2016.09.018
Pressure averaged 297.3 ± 120.0 kPa with no padding to 90.3 ± 38.2 kPa, and it maintained the strong offloading force for 3-4 days before diminishing.
Zimny S, Reinsch B, Schatz H, Pfohl M. Effects of felted foam on plantar pressures in the treatment of neuropathic diabetic foot ulcers. Diabetes Care. 2001;24(12):2153–4.
doi: 10.2337/diacare.24.12.2153.
If a practitioner wishes to consider using felt, it's worth noting its advantages and disadvantages relative to other offloading techniques.
Some advantages to using accommodative felt to offload a wound are:
-
Felt works. There aren't a lot of studies out there on felt (there's not as much funding compared to expensive medications and bandages). But in two reasonably good studies, 78-81% of ulcers healed within 12 weeks, making it one of the more effective treatments.
-
As felt is usually attached to the foot (though sometimes to an innersole or shoe), It is one of the few offloading techniques that addresses shear--that is the movement of the foot within an offloading product like a shoe or boot.
-
Felt is inexpensive.
-
It doesn't require a sophisticated skill set to apply.
-
It's not as bulky as some of the other forms of offloading discussed below, so it's not uncomfortable and doesn't make the foot unstable.
-
It has the benefit of staying on the foot even when the patient isn't wearing a shoe.
-
The patient can drive with it.
-
It doesn't lift the treated leg excessively throwing off the opposite limb. So it doesn't typically tend to irritate the back or make walking difficult or unstable.
-
The patient and clinician can also keep an eye on the foot for signs of infection or discharge with this technique.
-
Patients tend to be compliant with it, and don't typically remove it.
-
It's easily removed if there is a problem of some sort.
-
And it can be coupled with other forms of offloading, to augment the effectiveness of offloading
Some of the downsides to using accommodative felt to offload a wound are:
-
There is some time and labour involved with its application. Many clinics would prefer to hand a patient an off-the-shelf offloading shoe and move on to the next patient.
-
The padding can compress or slide, which can make it ineffective.
-
It can create new pressure issues at the edge of the pad, if not cut and applied correctly.
-
The patient can't get the foot wet, as the padding will absorb water. (Though one doesn't usually want the wound to get wet anyway.)
-
As a rule, thicker padding is more effective than thinner felt padding. However, it can be hard to source padding that is thick enough.
-
Accommodative padding works better for simpler ulcerations on the ball of the foot or great toe than ulcers in the midfoot or rearfoot.
Our Bottom Line on Accomodative Felt Padding:
By itself, padding is not statistically the most effective way to offload a wound. That honor is reserved for non-removable offloading systems such as the Total Contact Cast (TCC) or a non-removable offloading boot, both of which are discussed below.
Nonetheless, accommodative felt dressings can be extremely effective if applied correctly, particularly for simpler wounds located in the forefoot, or in wounds where other options of offloading are contraindicated for some reason. Further, it's easy to use, it's cheap, and it offers a high degree of acceptability to most patients.
In our opinion, felt often doesn't work as well for midfoot or rearfoot wounds.
And generally speaking, when this method is employed, the preference is to couple it with offloading footwear, as discussed below.
Off-the-Shelf Shoes and Sandals & Customizable Innersoles
A variety of footwear products have been used for foot ulcers. And they've been shown to work with most forefoot ulcers.
Birke JA, Pavich MA, Patout CA Jr, Horswell R. Comparison of forefoot ulcer healing using alternative off-loading methods in patients with diabetes mellitus. Adv Skin Wound Care 2002 Sep-Oct;15(5):210-5.
Perhaps the simplest is a standard surgical shoe.

While some physicians use a surgical shoe as its own offloading tool, a surgical shoe like the one above is rather ineffective at offloading wound. It should be used with a customizable, offloading innersole. We'll discuss the shoe first, then discuss an appropriate innersole.
A surgical shoe like this one uses a velcro closure that can be easily adjusted for the thickness of a bandage and a customizable innersole. This makes it very easy to use in a patient with significant swelling or deformity as seen with Charcot.
The sole of the shoe does not bend like a regular shoe, which can decrease pressure and strain of bending of the joints in the ball of the foot during gait.
The heel height is made to be similar to a regular shoe on the opposite limb, making it easy on the back.
And the sole has good grip, making them suitable for use in Canadian winters.
Another benefit of a shoe like this is that it is removable for sleeping. The patient doesn't have to wear a dirty shoe that's been on the street to bed.
They're also cheap enough that patients will often choose to buy two--one for inside the house, and one for the street.
But its being removable is also a downside. Because it can be removed, it often is, and patients may not always use it when weight bearing. They may not put it on because, "I'm just going to the bathroom" or "I'm just going to the kitchen."
So only very compliant patients can use this effectively.
But this shoe does not, by itself, offload a wound effectively. The innersole a surgical shoe comes with is not customizable, nor does it offload a wound. Thus a shoe like this needs to be coupled with an offloading innersole of some sort.
There are several types of customizable innersoles for a shoe like this.
One of the most common innersoles used in a shoe like this consists of several layers of foam. Plugs can be removed from the bottom of the innersole, creating a hole in the area of the ulcer, meant to offload the ulcer. The idea of this makes intuitive sense.


But the quality of some versions of this style innersole can vary.
Some of these innersoles flatten out rather quickly, and sometimes adjacent plugs become loose and fall out, expanding the size of the desired hole, diminishing the effectiveness of this innersole as an offloading device. Thus, they may need continual replacement.
To the right we see an example of an innersole that has flattened over just 4 weeks of wear, with the plugs adjacent to the desired hole having fallen out. The result is a hole is 3x larger than it should be, much too large for the ulcer site--one that does nothing to offload the ulcer.

The innersole to the right has a similar design. It, too, is breaking down--in this case after 6 weeks of wear.
At this point, the degree of effective offloading is minimal.

The FORS innersole was developed in Venice, Italy, and operates by a similar principle.
It also has plugs that can be removed to offload a wound, and it's been shown that this diminishes pressure by an average of 43%, which appears to be at least as effective as other offloading innersoles described above.
McGuire J, Furmato J, Borys J. Evaluation of a pixelated innersole designed to offload areas of elevated pressure on the sole of at-risk feet. Poster presented at American Podiatric Medicine Association Annual Meeting 2017.


Without a proper study, it is difficult to state that they make offloading more effective.
What we can say is that these innersoles are are well made. They're more substantial and thicker than most of the others available, and they're made of a different material--Poron instead of foam.
The different material means that they appear to last well longer than other innersoles, and the adjacent plugs don't come loose and fall out.
To the left is a FORS innersole after five months of every-day usage.
Compare how well this has held up compared to the examples above, which were useless by week 4-6.
Of the innersole systems we've tried, this is our favourite. (And no, we are not sponsored in any way by any company.)
Our Bottom Line on Surgical Shoes and Offloading Innersoles
A flat-soled surgical shoe like the one above with an innersole system like the FORS may work well to treat a smaller, simpler wound of the forefoot.
With this said, we tend not to use this on its own. We prefer to couple this system with an accommodative, felt dressing applied to the foot, as the felt diminishes shearing forces even within footwear with an offloading innersole.
No study combining a FORS innersole in a surgical shoe and an accommodative, felt dressing has been done, but it has been our experience that the combination improves wound healing success.
It is our opinion that it works better for smaller, simpler wounds of the forefoot, less well for midfoot and rearfoot lesions.
They need to be used in patients who can be trusted to be compliant. If the patient removes them because they're "just going to the bathroom," or "just going to the kitchen," they are often not used enough to allow for uneventful healing.
Healing Shoes and Sandals
Other offloading shoes on the market are offloading shoes and sandals. These shoes are better made and more substantial than those above--with a better heel counter that better controls side-to side movement (shear). These shoes are therefore more expensive.


To provide offloading, these shoes come with a set of customizable innersoles. In the example below, offloading is achieved not through the removal of plugs, but through apertures cut into the middle layers of the innersole system.


We have found shoes and sandals like these can be effective. Though when these shoes are used by the author of this webpage in the treatment of active wounds, the shoes and innersoles are coupled with an offloading felt dressing.
The shoes and sandals are well made, and the innersole system it comes with is pretty good. The quality will vary based on the brand of offloading shoe / sandal. We find the innersoles last longer than most peg-systems but not as long as the FORS innersole.
As with all removable offloading devices, they're dependent upon the patient to use with each and every step. Patients who cannot be trusted to wear these shoes religiously should be placed in a non-removable system like a Total Contact Cast (TCC) or a non-removable boot. Both are discussed below.
There are a few downsides to shoes and sandals. First, they are more costly than the simple surgical shoe we described above. But these are better made, may be easier to walk with, and many patients feel they're worth the added cost.
However, in order to fit in four innersoles, these shoes and sandals have to be deep. This means the soles are quite elevated, and they can be unstable for some patients, especially the elderly, the frail, and those who are unsteady with neuropathy or some other issue.
This is especially true when only one sandal or shoe is used at any one time, with normal footwear on the other foot. Thus using only one shoe on the foot with the wound along with a lower-height street shoe on the other limb can make it hard on the back. So most patients buy the pair of shoes, even if there is a wound on just one foot.
One other common complaint we find for our Canadian patients in winter is that the sole is quite smooth, making them less practical in the winter.
Our Bottom Line on Offloading Shoes and Sandals
The good: Very well-made footwear, ideal for those who want more lateral stability
than a surgical shoe can offer. They hold up well enough that some patients like them for the long term, even after the ulcer has healed.
The not-so good: The 4-layer offloading system that comes with the shoe is better
than some, but not as good as others, such as the FORS. The place the foot high, and can be unstable for some. The sole has minimal tread for winter.
Wedge Shoes
One footwear option commonly used in Canada are these wedged, half-soled shoes.
They can be made with the forefoot elevated (top right) to relieve pressure in the forefoot, or with the rearfoot elevated (below right) to relieve pressure in the rearfoot.
These shoes have a removable innersole, so one could use a customizable offloading innersole with it, like the one shown above. But most wound care facilities in our area seem to simply given out as is, with no customized innersole.
Some studies show these shoes can decrease the forces on an ulcer by up to 50%, and studies show healing rates of 44-58% at 12 weeks.
So they're helpful and have an advantage of not requiring much time of the treating clinician. However, they come with some downsides.
For example, they're quite a bit elevated compared to normal shoes, or to the flat surgical shoe above. They make one limb higher than the other, which can be uncomfortable for the back.
Further, the cliff-edge design can make transfer of weight forward jarring and clumsy. They can make the patient unstable, and more prone to falls--particularly in a neuropathic patient who may be more unstable than normal.
They're also hard to drive with.


Armstrong DG, Nguyen HC, Lavery LA, van Schie CH, Boulton AJ, Harkless LB.
Off-loading the diabetic foot wound: a randomized clinical trial.
Diabetes Care. 2001 Jun;24(6):1019-22. Erratum in: Diabetes Care 2001
Aug;24(8):1509. PubMed PMID: 11375363.
Off-the-Shelf Offloading Boots
There are off-the-shelf boots that can be used to treat wounds, as well. Externally, it looks virtually identical to the standard walking boots used to treat fractured bones, twisted ankles or similar conditions. However, the offloading version comes with an innersole of some sort (as shown above) that can be customized to offload an ulcer.
Many companies make these boots. On the left is a US device. We commonly use the one in the middle, which are imported from from Iceland. It features an air bladder to tighten the boot on the leg. On the right is a fashionable version from Italy.
Our Bottom Line on Wedge Shoes
Wedge shoes decrease pressure on an ulcer, and achieve healing in about half of patients at 12 weeks. But they're not as stable or as comfortable as the flat, surgical shoe with an offloading innersole or a boot (discussed below), and they're not as effective as a TCC, a boot, or felt.
We feel the reason wedge shoes are chosen is that they can simply be dispensed without customization as most facilities do not have practitioners trained for more customized options.



Walkers like these improve healing because, not only do they offload, but unlike the shoes above, they tend to shorten the patient's stride, and patients tend to take fewer steps when they're used. This makes the boots more effective than the shoes and sandals above.
Crews RT, Sayeed F, Najafi B. Impact of strut height on offloading capacity
of removable cast walkers. Clin Biomech. 2012;27;7:725.
In their removable form (which is how the vast majority of these boots are used), the healing rates range from 52-65%, with some numbers in this range a fair bit lower than expected because patient compliance is typically poor.
Further, they're bulky, they're slow for patients to put on and take off, they alter one's gait, and, they're not conducive to driving. Thus, compliance is often poor. Many patients who are prescribed a boot like this use them for between 28%* and 59%** of steps taken during the day.
*Armstrong DG, Lavery LA, Kimbriel HR, et al. Activity patterns of patients with
diabetic foot ulceration: Patients with active ulceration may not adhere to a
standard pressure off-loading regimen. Diabetes Care. 2003;26:2595.
**Crews RT, Shen BJ, Campbell L, et al. Role and determinants of adherence to
offloading in diabetic ulcer healing. A prospective investigation.
Diabetes Care. 2016;39:1371.
If the patient's boot is made so that it is not removable with a cable tie--a so-called instant total contact cast or iTCC--the healing rate is sharply improved. In fact, with a cable tie, the healing rate of these boots is very nearly as good as the total contact cast discussed below--in the 85-90% range. This would make them the 2nd most effective way to offload an ulcer.
However, they're rarely made non-removable by the clinic that dispenses them.
Katz IA, Harlan A, Miranda-Palma B, Prieto-Sanchez L, Armstrong DG, Bowker JH,
Mizel MS, Boulton AJ. A randomized trial of two irremovable off-loading devices
in the management of plantar neuropathic diabetic foot ulcers. Diabetes Care.
2005 Mar;28(3):555-9. PubMed PMID: 15735187.
Our Bottom Line on Offloading Walking Boots
A removable walking boot can be excellent offloading option in a motivated, compliant patient.
In a non-compliant patient, using a cable tie renders the boot non-removable, making the healing rate climb to Total Contact Cast levels.
However, boots like these aren't perfect. They're bulky, clumsy, warm, and hard to drive with.
As total contact casts, long considered the best offloading option, remain underused in wound clinics because they're expensive and time consuming to remove and apply, a walking boot made non-removable may be a viable option.

Total Contact Cast (TCC)
A total contact cast or TCC is a specially-designed cast used to treat neuopathic wounds and Charcot neuroarthropathy.
The TCC redistributes weight from the wound, sheltering it from the pressure and sheer forces that create ulcerations.
They're somewhat awkward and clumsy. On the plus side, this means patients using them take shorter steps and fewer steps. They're typically changed weekly.
The big benefit to a TCC is that the foot is kept safe and sheltered from the pressure and sheer forces that create ulcerations. TCCs simply work better than anything else, making it the gold standard in offloading neuropathic foot ulcers.
For this reason, TCCs have long been this author's favorite method of offloading difficult wounds, and wounds of the midfoot and rearfoot.
TCCs are so effective that several authors report 85-90% healing rates within 6-8 weeks. Below we see a chart of nine studies showing the healing rate of ulcers treated with a TCC.


Ulcers also heal pretty quickly with a TCC. If we compare the results of twelve studies from several different countries, TCCs heal ulcers in an average of 39.1 days or 6 weeks, with most studies falling into an average of between 5 and 8 weeks.
.png)
Crews RT, Girgis C, Domijancic R, et al. Influence of offloading induced limb length discrepancies upon spinal alignment. Presented at the 2017 American Diabetes Association Annual Meeting; June 22-26, 2018; Orlando, FL. Abstract 104-OR.
Wu SC, Jensen JL, Weber AK, et al. Use of pressure offloading devices in diabetic foot ulcers: Do we practice what we preach? Diabetes Care. 2008;31:2118.
So if TCCs are so great, why doesn't everybody use them?
TCCs are used somewhere between 5 and 10% of wound care clinics in North America. And even though they are this author's favorite way to offload a severe wound, we don't use them for most of our ulcer patients.
There are several reasons they're not used frequently.
-
First, TCC application requires a degree of specialized training. And training people to apply TCCs is not something our government health systems appear to be prioritizing.
-
Casts are relatively expensive, and they're typically removed and reapplied weekly, adding to the expense. While a case could be made that healing severe wounds quickly saves money and saves limbs, this cost is nonetheless not typically covered by most Canadian provincial health programs.
-
Some podiatric wound specialists apply them, but they are mostly private-paid.
-
TCCs are time consuming to put on and take off, particularly if the clinician doesn't have a lot of experience with them.
-
TCCs have the potential to cause harm--abrasions, pressure--that can create new ulcers, particularly if the foot and leg swells a lot or if it's improperly applied. This is not a major problem in most cases, however, particularly for practitioners who apply a lot of TCCs.
-
You also can't use it with infected wounds, and you might miss new infections while the patient is sealed up in a cast.
-
TCCs can also be unstable for the elderly and those with balance issues.
-
It's impossible to drive with a TCC on the right foot.
-
Those sensitive to claustrophobia may not enjoy a TCC.
-
You can't bathe easily with it.
-
It can be cumbersome to sleep with a TCC.
Nonetheless, TCCs do have success rates higher than any other offloading technique, and if you have a difficult wound, particularly in the midfoot or rearfoot, it may be the treatment of choice.
To learn how they're put on the foot, we have a page on the application of a Total Contact Cast here.
Our Bottom Line on Total Contact Casts (TCCs)
Multiple studies show that TCCs are the most effective offloading option, the gold standard, with healing rates of approximately 85-90%, and often at a quicker pace. In our practice, TCCs are usually the first choice for midfoot wounds, for rearfoot wounds, and for wounds that are non-responsive to other offloading techniques.
There are some contra-indications for TCCs, and you can't use them on every ulcer patient, such as infected wounds and in unstable patients.
Further, there are times when other offloading methods may be preferable because they also very likely to work and have benefits of being simpler, more economical, and more practical in terms of function in every day life.
So what's the best offloading methods?
When we compile data from these various studies, (below), we see that total contact casts heal ulcers more effectively and more quickly. Non-removable boots are 2nd best, followed by offloading with simple felt.
Removable knee-high boots are next, with various shoes and ankle boots healing in roughly the same range.
Dressings, by themselves, are by far the least likely to heal, with healing rates less than 1 in 3 and over an extended timeline.
(Healing rates below are at 12 weeks.)

TCC = Total Contact Cast
NRWB = Non-Removable Walking Boot
RWB = Removable Walking Boot
Another option we use most commonly is to combine offloading techniques.
In the case to the right, for a slow-healing ulcer on the lateral (outside border) of the heel, we used two layers of 1/4" felt (approximately 80% healing rate by itself) combined with a customizable offloading innersole used in a knee-high removable walking boot (approximately 60% healing rate by itself).
There aren't many studies on combining offloading techniques, but it makes sense that it should be more effective than either modality is by itself.

Our Bottom Line:
1. TCCs are statistically the best option. But they're costly, time-consuming, and most facilities don't apply them routinely. The author uses them mostly for rearfoot ulcers and non-responsive ulcers.
2. Non-removable offloading techniques of any sort (as shown by the darker red bars in the chart above) consistently show greater success in healing wounds that removable offloading. Of these, felt is the easiest and cheapest alternative.
3. For routine forefoot ulcers, we commonly combine 1/4" to 1/2" offloading felt with surgical shoes or below-the-knee boots and FORS innersoles. We have found the FORS innersoles to be more comfortable to walk in and more stable than wedge shoes and have found them to be more durable than most foam-peg systems.
There is no study published that has examined this combination of offloading, but our experience has found 85-90% success for forefoot ulcers, which compares favourably to a total contact cast at a lower cost.
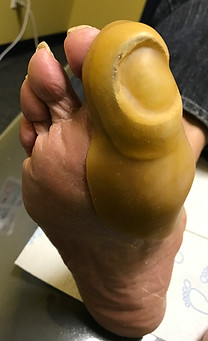
4. For digital ulcers, we commonly use surgical offloading, discussed on this site, and MPC (moldable podiatric compound or Berkoplast) for patients who are not surgical candidates.
5. Even complicated wounds can heal with offloading, as seen in the examples below.






Long-Term Offloading
Once the ulcer is healed, there is a need for long-term offloading, otherwise the wound tends to return. There are various devices that can offload a toe ulcer long-term.
For toes, often simple digital offloading devices are more helpful than more expensive inserts or shoes. For digital ulcers, simple surgical options are often very helpful too, which we discuss here.
CROW Boot
A CROW boot (CROW stands for Charcot Restraint Orthotic Walker) is a custom-made boot similar in external appearance to an offloading boot like those discussed above, but it's custom made, and the inside is more similar to a TCC.
In theory, the CROW should be as safe and comfortable as a TCC, but unlike the TCC, a CROW boot is removable.
The benefit to a CROW boot being removable is that it allows the patient to take it off at night to sleep or to bathe.
The downside is that the patient may take it off and not use it consistently. It's also takes some time to make--sometimes the ulcer is healed by the time the CROW is ready. And as a CROW boot is custom made, it can be rather costly.
For these reasons the CROW is often reserved more for Charcot neuroarthropathy, which may create chronic, severe deformities and ulcerations, than for a routine neuropathic ulcer.
But these can be quite helpful to treat ulcers as well, particularly in difficult wounds, or as a long-term offloading option for patients with significant deformity that cannot be accommodated in traditional footwear.
In the photo to the right the CROW is worn by a patient who worked as a professional chef. The CROW allowed the patient to continue working in a job that he really shouldn't have been doing at all, given his condition.


Our Bottom Line on CROW Boots.
CROW boots are costly and take time to make, so they're not practical to treat most
wounds.
They may be a very good option for slow-healing wounds, or as a long-term offloading
option for certain wounds with an unstable or problematic foot structure.
They're excellent options for Charcot patients with significant deformity, who need longer-term offloading
options.
Ulcers in the ball of the foot, arch or rear foot may be offloaded through an orthotic with an accommodation (depression) built in (below left), or through a custom shoe (below right is a custom, steel-toed work boot), with similar offloading built in.



What about getting all the patient's body weight off the wound?
For instance, a wheelchair could offload a wound completely.
The downside is that it's not convenient or practical for patients, and not really healthy for a patient to sit for weeks on end while a wound heals. And it may not be healthy for the skin either, as there is some evidence that being completely immobile may cause the skin to atrophy and weaken, making future ulcers more likely.
Crutches could completely offload a wound, too. But they
can be uncomfortable and unstable for many. Further, there
is a significant tendency for patients to be non-compliant
and use the crutches only intermittently.
They're more likely to be effective for younger, fitter
patients, but younger, fitter patients are not typically those
who present with a wound. Thus we rarely recommend
crutches to offload a wound.
There are kneeling scooters (right) that can be used for
complete offloading. These are often more stable than
crutches, and we do recommend them in patients who
need complete offloading, in those we trust to be compliant,
and those stable enough to use them.
However, the continued pressure on the knee and lower leg
can prove uncomfortable.
While techniques to completely offload the foot are sometimes necessary, but when possible, we try to keep the patient offloaded while still able to walk.
Surgical Offloading
Ulcers may be offloaded for the long-term through surgery--procedures designed to diminish the pressure and shearing forces that cause the wound to form in the first place.
In many cases surgical intervention can be the safest and most successful way to offload a wound to get it to heal, and to keep it healed.
This is a big topic, so we've devoted other pages to the concept of surgical offloading.
To visit other pages involving the treatments of wounds, click on debridement, treating infection, bandages and dressings, and specialized treatments.
To return to the top of the page,
click on the maple leaf to the right.
This page written by Dr. S A Schumacher
Podiatric Surgeon
Surrey, British Columbia Canada
Unless otherwise indicated, all clinical photographs owned and provided by Dr. S A Schumacher. They may be reproduced for educational purposes with attribution to: Dr. S A Schumacher, www.canadianmaple.org

