

Canadian
maple
Medical Alliance for the Preservation of the Lower Extremity
Dermatology
of the Diabetic and Renal Patient
Many diabetic patients develop abnormal changes in the skin. In fact, one study found skin changes developed in 84% of diabetic patients.
Furqan S, Kamani L, Jabbar A. Skin manifestations in diabetes mellitus. J Ayub Med Coll Abbottabad. 2014 Jan-Mar;26(1):46-8.
“A warrior is defined by his scars, not his medals.”
-- Matshona Dhliwayo
Change in the skin of diabetic and renal patients can be a result of altered circulation, neuropathy, endocrine changes, autoimmune disorders, inflammation, infectious disease, deteriorating structure, changes in biomechanics, and systemic disease.
Let's begin with Changes in Moisture.
Perspiration is controlled by nerves, and this can be affected by autonomic neuropathy.
Occasionally, as seen to the right, diabetic patients develop an increased in moisture content (maceration) through an increase in perspiration (hyperhidrosis). This is amplified when the foot is kept in heavy socks and shoes for periods of time.
In the two examples to the right, most of the excessive moisture is caused by the moisture content created by the wound. Our bodies are mostly water, so when the skin is open, moisture leaves the body.
High moisture content can weaken the skin and lead to ulceration and infection.
Wound dressings are important in cases like this to help dry the foot and prevent further skin deteriorzation and infection.




Much more commonly, as seen in the images to each side and below, diabetes leads to excessively dry skin.
This is also known as xerosis or xeroderma. (The 'x' in these words is pronounced as a 'z', so it's pronounced zerO-sis and zero-DER-ma). You see examples to each side and below.
Dry, cracked skin may lead to fissures and bleeding. The skin becomes weaker and less resilient to pressure and shear, which may lead to ulcerations, and bacterial infections.
Sometimes infections get out of hand, particularly so in diabetics. And this can make the patient more susceptible to amputation.
Examining the foot daily to monitor for any breaks in the skin and maintaining proper moisture balance by wicking away fluid, regular changes in socks and shoes in the damp foot, and applying moisture the foot with excessively dry skin is vital.




The skin on the legs can also become thin and shiny and waxy in appearance. There can also be loss of hair in the legs and feet, both from diminished circulation that often accompanies diabetes, and the diabetes itself. Changes in the skin of this nature affect approximately half of diabetics, becoming more common with time.
Source:
James, William D.; Berger, Timothy G.; et al. (2006). Andrews' Diseases of the Skin:
Clinical Dermatology. Saunders Elsevier. ISBN 0-7216-2921-0.
Fungal Infections of Skin and Nails
Thin, cracked, weakened, compromised skin can also make a diabetic susceptible to fungal infections of the skin. This is known as tinea pedis, or more colloquially as athlete's foot. The fungus is often dry, white, and peeling.

Certain fungal infection (particularly Trichophyton rubrum) may make the skin red and itchy.

With time, fungus may spread from the skin to the nails, making the nails, thick, discolored and misshapen. And the nails can harbour the fungus, making reinfection of the skin a frequent, recurrent event.
The nails can become quite thick, misshapen and difficult to maintain, particularly when many diabetics are older and have difficulty bending.
And many diabetics, and older people generally, have difficulty seeing their feet, making difficult even routine footcare tasks--like washing the feet, cutting the nails, and keeping the feet properly moisturized.

This commonly leads to the nails and skin getting out of control.

Ingrown Nails
Ingrown nails are a common complaint with or without neuropathy.
In most patients, the ingrown nail looks somewhat like the image to the right. The nail is stabbing the skin; the skin swells and becomes reddened.
.jpeg)
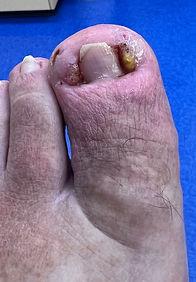
In neuropathic patients, sometimes the nails become more inflamed and angry looking as the issue may not have been noticed right away.
The red, angry tissue is called granulation tissue. It represents the body's attempt bring increased blood to the tissue to help the toe heal, but because the nail is still present, it grows up and around the nail.


When the condition persists long enough without attention, the inflamed, swollen granulation tissue becomes a permanent-looking feature.
Ingrown nails can be addressed permanently in a straight-forward way. The problematic nails can be cut back and those sides can be permanently cauterized in some way (chemical, radiosurgical, electric, mechanical cautery) so they never grow back. In the near photograph, you can see how it is usually done; on the right sutures were used to remove all the granulation tissue.


To the right is a nail that is fully healed from the procedure.

Bruising and Infections
Thin, dry, neuropathic skin can also make a diabetic's skin more fragile and susceptible to injury. This is often seen as bruising, which may occur with little in the way of trauma.
But if the skin is compromised enough to breach the barrier, bacterial infections may develop. This is quite common in neuropathic patients who cannot feel the damage being done to the feet. Before the patient to the right removed his foot from his sock, he had no idea there had been any injury to the foot.
The patient pictured below left could not recall any injury to his leg other than scratching an itch.
Below center, the damage to the toe resulted from simply wearing a shoe that rubbed the top of the toe. The damage was significant enough that the toe became dusky. This led to gangrene and amputation of the digit. Note the tight, thickened, inflexible skin known as sclerosis. This will be discussed below.
The patient below right simply leaned against a rung of a ladder.
Injuries like these exhibit significant injury from what a non-neuropathic patient would find incidental and non-injurious.

_JPG.jpg)


Calluses and Corns
Diabetic motor neuropathy may often result in crooked toes, prominent bones, and
abnormal gait, and this can produce sites of abnormal pressure and friction. This may result in areas of thickened dead skin. Depending upon their location, these areas of thickened dead skin build up are known as a corn or callus. (The word "callous" is the adjective form--as in calloused skin or a callous person.)
In those patients with sensory neuropathy, the patient may not feel or notice corns
and calluses developing, and they can become quite thickened. If bad enough, the
callus or corn may create an ulcer (hole in the skin), as discussed below.



Ulcers
When sensory loss (sensory neuropathy) is present, the thickened skin of corns and calluses (above) can begin to tear the living skin below, and an ulcer may develop (right).
The patient may not be able to feel the damage that creates the ulcer, and the damage may become significant. Ulcers may put the patient at risk of infection of the soft tissues or bone. This may result in lengthy and expensive treatments. They may sometimes lead to amputation and premature death.
Ulcers are, of course, the main topic of this website, and there are many
photographs of ulcers throughout.
To learn more about abnormal biomechanics associated with wounds, click here. To learn how the skin breaks down to form wounds, click here.

Diabetic Dermopathy (Shin Spots)
Diabetic dermopathy (pronounced derm-AH-path-ee) is a disorder of the skin that results in brown or, less frequently, pinkish discolorations of the skin. They're usually round or oval, and tend to develop on the front (anterior portion) of the legs.
While the medical literature gives a wide range of prevalence, it's safe to say this is one of the most common skin pathologies that develop with diabetes.
Microscopic examination demonstrates altered microcirculation, a leakage of blood contents into the skin, and an increase in melanin (the component of skin that provides pigment).
Diabetic dermopathy is more common in those who have had diabetes for several years, and in those with poor sugar control. They are more likely to be associated with more severe neuropathy, retinal disease and kidney disease, so the presence of diabetic dermopathy should raise a clinical suspicion of these other pathologies.
The lesions, themselves, do not typically hurt, they don't ulcerate, and the discolorations do not need to be treated.



Good sources on diabetic dermopathy:
Rapini, Ronald P.; Bolognia, Jean L.; Jorizzo, Joseph L. (2007).
Dermatology: 2-Volume Set. St. Louis: Mosby. ISBN 1-4160-2999-0.
James, William D.; Berger, Timothy G.; et al. (2006). Andrews' Diseases of the Skin: Clinical Dermatology. Saunders Elsevier. ISBN 0-7216-2921-0.
Morgan, AJ, Schwartz, RA. "Diabetic dermopathy: a subtle sign with grave implications". J Am Acad Dermatol. vol. 58. 2008. pp. 447-51.
Kiziltan, ME, Benbir, G, Akalin, MA. "Is diabetic dermopathy a sign for severe neuropathy in patients with diabetes mellitus? Nerve conduction studies and symptom analysis". Clin Neurophysiol. vol. 117. 2006. pp. 1862-9.
Abdollahi, A, Daneshpazhooh, M, Amirchaghmaghi, E, Sheikhi, S, Eshrati, B, Bastanhagh, MH. "Dermopathy and retinopathy in diabetes: is there an association". Dermatology. vol. 214. 2007. pp. 133-6.
Brugler, A, Thompson, S, Turner, S, Ngo, B, Rendell, M. "Skin blood flow abnormalities in diabetic dermopathy". J Am Acad Dermatol. vol. 65. 2011. pp. 559-563.
Shemer, A, Berman, R, Linn, S, Kantor, Y, Friedman-Birnbaum, R. "Diabetic dermopathy and internal complications in diabetes mellitus". Int J Dermatol. vol. 37, 1998. pp.113-115
Romano, G, Moretti, G, DiBenedetto, A, Giofre, C, DiCesare, E, Russo, G. "Skin lesions in diabetes mellitus: prevalence and clinical correlations". Diabetes es Clin Prac. vol 39, 1998. pp.101-106
McCash, S, Emanuel, PO. "Defining diabetic dermopathy". J Dermatol. vol. 38. 2011. pp. 988-92.
Uremic Hyperpigmentation
Uremic hyperpigmentation, found in some patients with chronic kidney disease and end-stage renal disease and dialysis patients, can appear similar to diabetic dermopathy. It also appears on the lower legs, although it often exhibits a wider distribution such as the calves and ankles.
While diabetic neuropathy develops brown spots, uremic hyperpigmentation is a more diffuse, brown or bronze discoloration, a result of impaired renal clearance.
Skin texture may be dry and itching may be present, but the skin is not inflammatory, it does not ulcerate, and is considered benign.



Although the world is full of suffering,
it is also full of overcoming it.
--Helen Keller
Post-Inflammatory Hyperpigmentation
Another form of hyperpigmentation develops after chronic inflammation. This is known as post-inflammatory hyperpigmentation, and is a result of hemosiderin deposits in a foot with diminished circulation, chronic micro-trauma and inflammation.
Note the neuropathic ulceration on the bottom of the foot at the base of where the 5th the should be.


Acquired Ichthyosis from renal failure
Acquired ichthyosis is associated with renal failure (and other conditions like lymphoma and HIV).
Polygonal scales on the extensor surfaces may develop as a result of impaired lipid metabolism and diminished sweat and sebaceous gland activity. Uremic compounds accumulate.
The condition can improve with dialysis optimization or renal transplant. Treatment involves emollients and keratolytic agents.



Vitiligo
Vitiligo (vih-till-EYE-go) is a skin disorder where patches of the outermost layer of skin (epidermis) loses its natural pigment (melanin), and the skin becomes white. The cause is unknown, but a leading theory is that the cause may be autoimmune.
One does not have to be diabetic to develop vitiligo, but it is somewhat more common in diabetics, particularly Type 1 diabetics. Vitiligo typically involves the trunk or face, but may involve the lower extremity.

Necrobiosis Lipoidica
Similar to, but much rarer than diabetic dermopathy, Necrobiosis Lipoidica (NL), sometimes known as Necrobiosis Lipoidica Diabeticorum (NLD), also causes spots on the skin, and also most common in the anterior portion (front of) the lower leg.
Necrobiosis lipoidica lesions usually begin as isolated plaques, but may coalesce into larger regions.
Lesions can be inflamed, itchy and uncomfortable. If they progress, NL lesions may ulcerate.


The two photos above appear courtesy of www.hasshe.com

Dermatitis
Dermatitis is inflammation of the skin, often causing redness, irritation, and itching.
There are a variety of things that can cause dermatitis, as we'll see in this section.
Anyone can get dermatitis, but it dermatitis is more common in neuropathic individuals, as neuropathy may reduce moisture content in the leg, as shown above. This may make them itchy.
Peripheral neuropathy can also lead to abnormal sensations that can cause patients to scratch the skin, increasing inflammation, (right).
Eczema / Eczematous Dermatitis
Eczema is essentially a subtype of dermatitis.
Eczema features erythema (redness), scaling and flaking of skin, irregular, ill-defined borders, surface crusting, and thickening of skin (lichenification).
Venous Stasis / Dermatitis
Diabetics and renal patients often develop venous insufficiency. This may be a result of obesity and reduced mobility.
This, combined with peripheral neuropathy, can cause a diminishment of muscle pump function in the calf, lowering blood return to the heart, combining with gravity to stagnate fluids in the legs.
Neuropathy can also alter vascular tone. Blood vessels may become more dilated, further increasing fluid pressure.
Dialysis patients also have repeated swelling cycles in the legs that can strain the veins further.
When chronic venous insufficiency develops, the skin can become inflamed. The skin appears bright pin / red because the dominant process is acute inflammation and vasodilation. The capillaries open up and more oxygenated blood flows through the skin producing a brighter color. This is the Dermatitis component of Venous Stasis.
In the example to the right, there is yellow crusting from dried serous fluid (the tissue's fluid mixed with proteins) that has seeped through the skin.





To the right is a more advanced stage of venous stasis dermatitis.
Long-term inflammation has resulted in the skin turning darker, reflecting persistent inflammation, decreased oxygen, and venous congestion of the small blood vessels in the skin.
Red blood cells leak into the skin and become stagnant. The oxygen being transported by the blood cells bonds with the iron in the red blood cells creating hemosiderin deposits, a fancy way of saying rust. These are represented by the early formation of brown spots.
In chronic cases, like the example to the right, the swelling and seepage into the skin has been present for so long, the fluid so stagnant, the hemosiderin deposits becoming more widespread that the skin looks increasingly brown in colour.


If the skin stretches enough, water can begin to seep through the skin.
When enough water and proteins seep through, a venous ulcer may form.
Venous ulcers are usually located around the inside of the ankle.
This image shows a venous leg ulcer producing a large amount of wound drainage, as fluid leaks from the blood vessels and surrounding tissues.
The yellow-orange fluid is exudate, a mixture of serum, proteins, inflammatory cells and fibrin.
Venous ulcers commonly produce significant drainage until the swelling and venous pressure is controlled, usually with compression therapy.

In many cases, the wound becomes chronic. They slough becomes touch and hard.
Part of treatment involves trying to convert this tough tissue into fresh granulation tissue with young, active cells that can heal the wound.

The wound is usually healed with compressive stockings. The red tissue is granulation tissue, new tissue with blood vessels forming to repair the wound.
The skin is dry and scaly from the underlying venous disease.

Pruritus
Pruritus refers to itching. Diabetics may get this from having dry skin or a fungal infection.
It is seen with edema as well, where the skin is stretched, the water in the leg enters the skin, which sets off inflammation and itching (near right).
We see uremic pruritus with chronic kidney disease, especially those on dialysis (far right). It may be local or widespread. The skin appears dry, irritated, darkened, with scratch marks, scabs, or sores from repeated itching.


Gout
Gout is a condition caused by high levels of uric acid in the body. When uric acid builds up, it can form sharp crystals that settle in joints--most commonly in the cooler portions of the body such as the feet (classically the big toe as seen to the right and below), but it is common in the other toes and even the ankles and knees.
It commonly causes sudden episodes of pain--often severe--often swelling the joints. The area is often very warm.
Gout is very common in diabetics, but even more common in dialysis patients as the kidneys aren't functioning correctly and cannot remove the uric acid.


In many cases the white uric acid crystals become visible through the stretched, tight, and shiny skin as seen in the 3rd toe of the photo to the left.


When removed from the body, tophaceous deposits (clumps of uric acid) have a feta-cheese appearance.
Sclerosis
Sclerosis, a word of Greek origin means an 'abnormal hardening," and refers to thickened, tight, stiff skin.
Sclerosis is sometimes known as induration.
Sclerosis can be seen in a variety of locations, such as the leg to the right. But it is most problematic around joints, such as the ankles, knees, and elbows.
It is seen, too, in the digits of the body--both fingers and toes, as seen below), where it is known as digital sclerosis. The joints become stiff, less dexterous, less functional. In the lower extremity, it is sometimes accompanies the contractures of the digits caused by motor neuropathy. Stiff, sclerotic skin is more susceptible to injury.
Sclerosis may be seen as a result of gout (above), diabetes, chronic inflammation, infections, and a variety of other conditions.
In the cases below it is caused by chronic edema (swelling).



Diabetic Blisters (Bullosis Diabeticorum)
Occasionally diabetics may develop blistering, typically with no obvious cause. They may occur in multiples and may occur on either the upper or lower extremity but are more common in the foot. They are typically painless, and have no surrounding inflammation. They tend to resolve on their own, but healing can become an issue in patients with poor circulation or if they become infected.




Eruptive Xanthomatosis
Xanthomatosis (Zan-though-muh-toe-sis) refers to a group of lentil-sized bumps on the skin. They're typically yellow (xantho- means 'yellow' in Greek), but may also appear red or surrounded by a red border.
They consist of fat and cholesterol.


These two images appear courtesy of http://atlasdermatologico.com.br.
Disseminated Granuloma Annulare
Disseminated (meaning 'spread over a wide area') Granuloma (meaning 'inflamed vascular tissue') Annulare ('in a ring shape') refers to a skin condition meaning just that--a series of circular rings in the extremities.
They typically feature a reddish color, with a border.
These lesions do not necessarily require treatment. With time, they often fade on their own. However a variety of treatments do exist, including steroids, and light therapy.

This image appears courtesy of http://atlasdermatologico.com.br.

This image appears courtesy of http://epharmapedia.com
Gangrene
Diabetics will often develop poor circulation as a result of arterial disease that will often affect both large and small arteries. This is even more likely if the patient smokes or is on dialysis. It commonly presents as gangrene--the death of the tissue.
Gangrene may also be known as acral dry gangrene, where 'acral' refers to the periphery of the body (fingers and toes) and 'dry' refers to death of the tissue from blood loss and not as a result of infection.
The toes, being furthest from the heart, having very small blood vessels, and receiving a significant amount of trauma from walking, are often the first to exhibit the effects of circulation, as seen in these images.
Gangrene of the toes may involve a single toe (above right), a combination of toes (below left and center), or it may expand to extend up the foot, (below right).




While usually associated with the toes, dry, acral gangrene may also be present in the fingers (below left). This typically results in amputation (below right).


Gangrene in the feet must be differentiated from melanomas--an aggressive malignant condition of skin that also appears black, (right).


Calciphylaxis
Calciphylaxis is a rare but serious condition that occurs in some patients who are on dialysis or have advanced kidney disease, particularly those with diabetes.
In this condition, calcium deposits build up inside the small blood vessels in the skin, blocking blood flow to surrounding tissues.
Without adequate blood flow, the skin and underlying tissue begins to die, creating painful, dark, mottled patches, open, non-healing wounds and black scabs (eschar).




To return to the top of the page, click on the leaf to the right.
This page written by Dr. S A Schumacher
Podiatric Surgeon
Surrey, British Columbia Canada
Unless otherwise indicated, all clinical
photographs owned and provided by
Dr. S A Schumacher. They may be reproduced for educational purposes with attribution to:
Dr. S A Schumacher
