

Canadian
maple
Medical Alliance for the Preservation of the Lower Extremity
"It is just the feeling of a vacuum,
a void waiting to be filled."
--Eleanor Catton
The Rehearsal
Negative Pressure Wound Therapy (NPWT)
Negative Pressure Wound Therapy (NPWT), (sometimes called “vacuum-assisted closure”) is a treatment that uses gentle suction to help wounds heal.
A soft foam or gauze dressing is placed into the wound, sealed with an adhesive cover, and connected to a small pump that applies controlled negative pressure.
This suction helps remove excess fluid, reduce swelling, and draw the wound edges together, creating an environment that supports healing.
NPWT is most commonly used for larger, deeper, or post-surgical wounds, including diabetic foot ulcers, traumatic wounds, and wounds with heavy drainage. Studies show that NPWT can speed wound size reduction and promote granulation tissue, particularly when standard dressings alone are not sufficient. However, it is not a substitute for proper offloading, infection control, and blood flow, which remain essential for healing.
NPWT works best as part of a comprehensive wound-care plan rather than as a stand-alone treatment.
The technique begins with a specialized open-cell foamdressing, like those below, which is cut and shaped to fitthe contours of the wound. It is then applied directly to the wound. Sometimes gauze (below right) is used instead of foam.




The foam dressing is then covered by an occlusive plastic seal that adheres to the skin. A drainage tube extends from the dressing to a container, where the waste from the wound from the wound is deposited.

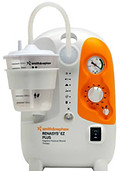
The vacuum is powered by an electric pump unit, such as those seen to the right.
When the vacuum is turned on, a negative pressure is created typically at -125mmHg, providing suction.





The suction may be applied continuously or, more commonly, intermittently.
NPWT is sometimes used with instillation--introducing fluids to flush through the wound. A variety of instillation products have been tried, such as antibiotic solutions, though evidence suggests that instillation with simple saline works just as well.
Kim PJ, Attinger CE, Oliver N, Garwood C, Evans KK, Steinberg JS, Lavery LA. Comparison of Outcomes for Normal Saline and an Antiseptic Solution for Negative-Pressure Wound Therapy with Instillation. Plast Reconstr Surg. 2015 Nov;136(5):657e-64e.
doi: 10.1097/PRS.0000000000001709. PubMed PMID: 26505723.
The dressing is changed about 2-3 times per week, more frequently if there is a lot of drainage or if the seal is damaged.
NPWT is generally considered useful for chronic wounds, acute wounds, traumatic wounds, burns, ulcers, flaps and grafts, and wound dehissence (where the wound edges are pulling apart).
NPWT is not used in the presence of malignancy, osteomyelitis (bone infection), necrotic tissues, over blood vessels, organs, nerves or unexplored fistulae.
How Does A Vacuum Help A Wound?
The vacuum has several positive effects on wounds.
First, the vacuum sucks away exudate, the fluid produced by the wound. This fluid is commonly filled with dead white
blood cells, pus, and other cellular debris that may inhibit
wound healing.
Second, along with the exudate, the vacuum removes bacteria, which are always present in a wound, continually trying to spread into the body.
"A vacuum is a hell of a lot better than some of the stuff nature replaces it with."
--Tennessee Williams
Third, the vacuum decreases edema and stagnant interstitial fluid (the fluid present between our cells). When there is a lot of this fluid, it can interfere with how well arterial blood, required for healing, is able to reach the wound.
Fourth, when the exudate is gone from the wound, new blood flow is drawn into the wound space by the negative pressure. Blood supplies the wound with oxygen, fresh cells, and the building blocks for proper wound healing.
Fifth, it maintains proper moisture environment. Wounds that are too dry don't heal well, and the vacuum promotes a moist environment conducive to healing.
Sixth, NPWT creates local changes at a microscopic level. The foam applied to the wound is made up of a firm, open cell material (a magnified example is seen below left). This foam bears down on the red, wound bed. When suction is applied through negative pressure, the segments of wound bed between the black foam struts is drawn upwards (below right). The budding effect created by NPWT is known as microdeformation.


As the black foam struts hold down the red wound bed, the vacuum draws up buds between the black foam struts, promoting new capillary growth. This is known as microdeformation.
Seventh, microdeformation results in new capillary growth into the wound, (granulation tissue), promoting cell growth to fill the void of the wound.
Eighth, the suction of the vacuum not only draws the wound bed and circulation vertically up into the void of the wound, it also draws the wound edges together horizontally across the wound, gradually decreasing the circumference of the ulceration. This process is known as macrodeformation, an example of which is below.



Above is a wound before starting
Negative Pressure Wound Therapy
Here we see the left and right wound edges beginning to be drawn together from vacuum created by Negative Pressure Wound Therapy.
The wound is approaching closure. The drawing together of the wound edges is known as macrodeformation.
Evidence for NPWT
There are literally thousands of studies on negative pressure wound therapy, and hundreds for its use in the neuropathic foot. Suffice it to say that the vast majority of studies on NPWT show positive effects. An early example from the prestigious Lancet found more wounds healed with NPWT than with standard therapy, and the wounds healed faster, too.
Armstrong DG, Lavery LA: Negative pressure wound therapy after partial diabetic foot amputation. Lancet 2005; 366:1704-1710.

In the photo above we see a chronic ulcer of several years duration that had been non-responsive to earlier treatments.
In fact, there are enough studies out there on NPWT that we can look at many studies at once to draw conclusions over larger patient populations. As one example, a 2017 review looked at 691 studies, chose what they felt were the best eleven, all randomized controlled trials, totaling 1,044 patients. They found that compared with standard dressing changes, NPWT had a higher rate, shorter healing times, greater reduction of wound area and wound depth, and patients suffered fewer amputations. They also found NPWT to be more cost-effective than standard dressing changes.
Liu S, He CZ, Cai YT, Xing QP, Guo YZ, Chen ZL, Su JL, Yang LP. Evaluation of negative-pressure wound therapy for patients with diabetic foot ulcers: systematic review and meta-analysis. Ther Clin Risk Manag. 2017 Apr 18;13:533-544. doi: 10.2147/TCRM.S131193. eCollection 2017. Review. PubMed PMID: 28458556; PubMed Central PMCID: MC5403129.
Liu Z, Dumville JC, Hinchliffe RJ, Cullum N, Game F, Stubbs N, Sweeting M, Peinemann F. Negative pressure wound therapy for treating foot wounds in people with diabetes mellitus. Cochrane Database Syst Rev. 2018 Oct 17;10:CD010318. doi: 10.1002/14651858.CD010318.pub3. PubMed PMID: 30328611; PubMed Central PMCID: PMC6517143.
A recent Cochrane review, (produced by a group of non-biased individuals without a financial conflict of interest in the topic being researched), was performed with a desire to determine if the number of patients healed with NPWT and the speed of healing were improved with NPWT. They examined eleven randomized controlled studies of 972 patients. While critical of imprecision and potential bias of some of the studies reviewed, they concluded that NPWT "may increase the proportion of wounds healed and reduce time to healing."
Wynn M, Freeman S. The efficacy of negative pressure wound therapy for diabetic foot ulcers: A systematised review. J Tissue Viability. 2019 Aug;28(3):152-160. doi: 10.1016/j.jtv.2019.04.001. Epub 2019 Apr 10. Review.
PubMed PMID: 31056407.
A 2019 British review looked at seven studies produced between 2008 and 2018. As with the Cochrane review, the researchers had criticisms of the studies in the literature, such as small sample sizes, and that many studies did not use the preferred reporting trials. However, they found that "All the included studies reported that NPWT led to better clinical outcomes when compared to standard treatment."

Our Bottom Line on Negative Pressure Wound Therapy
We at Canadian MAPLE like, use, and recommend NPWT.
NPWT appears to speed the healing of wounds, and we have found it particularly helpful for difficult, non-responsive wounds, where patients have had difficulty in healing through traditional means. In these patients, NPWT often seems to kick start a healing response that is difficult for a patient's body to initiate on its own.
One small downside is that while the motors of the bedside NPWT units are not loud, they are not silent, and they can be distracting for some patients, particularly on the intermittent setting, where the motor is repeatedly turning off, then kicking back on. Some patients use music or white noise to mask the sound of the NPWT unit.
In our experience, NPWT is most useful in a hospital setting, where patients are kept relatively sedentary and the negative pressure seal can be monitored by nursing staff.
There are home versions of NPWT, an example is seen to the right, that employ a unit that has no motor. Instead, suction is initiated by pulling a plunger. For some patients, particularly patients with wounds on the top and side of the foot, locations that are less likely to be disrupted by weight bearing, these units can be very effective.
However, some may find the seal of the NPWT to be difficult to maintain when they are at home, walking, and carrying on with normal activities. This is particularly true when patients are more active, and especially when the ulcer is located on the bottom of the foot, where the seal is most likely to be disrupted by walking.
To return to the top of this page, click on the maple leaf to the right
This page written by Dr. S A Schumacher
Podiatric Surgeon
Surrey, British Columbia Canada
Unless otherwise indicated, all clinical
photographs owned and provided by
Dr. S A Schumacher.
They may be reproduced for educational
purposes with attribution to:
Dr. S A Schumacher
