

Canadian
maple
Medical Alliance for the Preservation of the Lower Extremity
Biomechanics And Ulcer Formation
Biomechanics is an entire specialty. There are many texts written about biomechanics of the foot alone. So it's a difficult topic to fully cover on a webpage.
However, biomechanics of the foot is an incredibly important subject in understanding how and where neuropathic wounds develop and how those forces can be addressed to close the wound and keep it closed. Unfortunately, biomechanics is too poorly understood even within medicine. Few medical specialties really delve into this topic--the obvious major exception being podiatric medicine.
"It's not about medicine. It's about mechanics."
--Dr. Paul Brand (1914-2003)
Pioneer in Neuropathic Wounds
So to emphasize a few of the basic concepts behind the biomechanics of ulcer formation, we will provide you with several common examples. We'd recommend any ulcer patient see a foot specialist with a good understanding of biomechanical concepts, however, as your biomechanical issue may not be depicted on this page.
1) The body has five metatarsal bones--one behind each toe. The "heads" of the metatarsals are what make up the ball of the foot. They can be seen in the x-ray below left, viewed from the top of the foot looking down, each numbered.
In some people, one of those bones is lower (plantarflexed) than the others. That lower bone would be more prone to pressure, and would be a possible ulcer spot. You see the 1st metatarsal involved, below right.

1
2
3
4
5

However, any of the metatarsals may be affected. Below left, we see the fourth metatarsal is lower than the adjacent bones, resulting in an infected ulcer. Below right, the fifth metatarsal is lowest, also resulting in an infected ulcer.


An orthotic or custom shoe may offload these pressure sites. Alternatively, surgery may be required to correct these deformities.
Some physicians are reluctant to consider surgery in these patients, many of whom have diabetes, poor circulation or some other health concern. The patient may not heal, they say.
This is a legitimate concern. However, it needs to be balanced by the risks of not doing something. Wounds have high recurrence rates, and the risk of future infections from those wounds, and the patient's likely diminished ability to heal from those wounds, or from later surgery, when the patient is at a more advanced age, often with more advanced disease needs to be considered. These are difficult decisions.
2) If one of those metatarsal bones is excessively long compared to the adjacent metatarsal bones, this, too, could cause excessive pressure to develop, creating an ulcer.
The longest metatarsal is usually the 2nd metatarsal, and this is one of the most common ulcer locations (right).

3) A bunion--where the metatarsal to which the big toe attaches is deviated--is another common factor in ulcer formation. As the 1st metatarsal drifts away from the rest of the foot, more pressure is exerted on the 2nd metatarsal bone, creating an ulcer there (below left). This is extremely common. So this is a second reason someone may develop an ulcer in the same location as seen above.
Less frequently, an ulcer may form on the side of the foot from shoe pressure (below left and below center), or the top of the foot (below right).


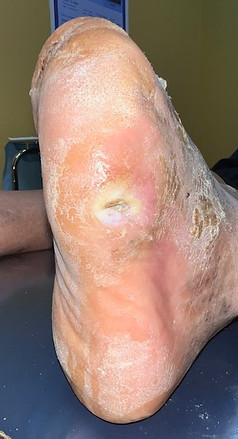

4) The side of the big toe is one of the most common ulcer sites.
Sometimes is occurs in a patient with a bunion, when the great toe is misaligned and weight is transferred off the side of the toe, and too much shear (friction) force develops at this site.
Other very common reasons an ulcer commonly develops here is when a person walks with an out-toed gait or when the foot pronates, or rolls inward excessively. The results often look the same.

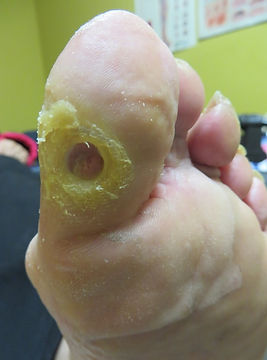



Above: An ulcer at the tip of the 2nd toe from a contracted, arthritic 2nd toe. The amputated 1st toe makes the smaller toes work harder, creating the deformity leading to the ulcer. This could be surgically corrected under local anesthetic, straightening the toe to prevent the ulcer's return.


5) Another reason the big toe is so commonly affected by neuropathic ulcers is when there is limited motion in the great toe joint. Below left you see a great toe that doesn't bend at all at the base of the toe (a condition known as hallux rigidus), hyperextending at the interphalangeal joint (the one nearest the nail) instead. Compare that to the photo of good toe joint motion, below right.
A lack of motion at the great toe joint causes the body to compensate, often by out-toeing and walking off the side of the foot, creating more pressure on the side of that great toe (as seen above). This can be corrected surgically, or sometimes controlled through orthotics or shoes, or ulcers tend to recur.
6) Hammertoes, where a lesser toe is contracted may result in an ulcer.
This is usually a result of the long tendons that flex the toes being recruited to stabilize the neuropathic foot, as seen to the right.
You can see how the toes contract to grab the ground, become misaligned and ultimately become deformed from this process.
Ulcers may then result from increased pressure, often at the tip of the toe, sometimes at the top, and sometimes between the toes.
Above: An ulcer at the tip of the 2nd toe offloaded with a moldable rubber instead of surgery. The ulcer resolved and has not returned in 4 years as of this writing.


Above: Here, too, the digits are contracted from trying to clutch the ground and provide stability. This has resulted in an ulcer so severe that the proximal phalanx bone is protruding through the wound.
Yet because of neuropathy, there was no pain. In fact, the patient was presenting to the hospital three times a week for dialysis and he never asked to have it treated as it wasn't bothersome.
To the right is a similar wound with exposed bone. The previous amputation of the great toe is likely a contributing factor here.
7) In gait, most people strike the ground on the outside (lateral) edge of the heel and transfer weight forward. Ulcers on the outside of the foot are common if heel strike or abnormalities in how the foot adapts to the ground develop.
In the example to the right, there is too much force on the outside of the foot, creating the ulcer beneath the small toe.

In this severe case (right), the foot has lost the function of the peroneal muscles that hold up the outside of the foot.
One can see how the outside of the foot is lower, and is more susceptible to pressure on that side of the foot.

8) A pronated foot, (right), where the foot rolls in excessively, is a common cause of ulcerations as well. This places more force on the bones on the inside of the foot (eg, the navicular, first cuneiform, the base of the 1st metatarsal) and creates a shearing (friction) as well, commonly causing ulcers on the side of the great toe or great toe joint.


This foot can develop complicated fractures in the midfoot that may lead the arch to collapse significantly, creating unexpected bony prominences in the arch of the foot.
9) There are times when the arch of a foot is collapsed for another reason. In the neuropathic foot, this collapse may be a result of Charcot neuroarthropathy (below). This foot can collapse significantly, creating complicated fractures and oddly-placed ulcers. This can be a very complicated foot to manage, particularly when it is not recognized early.


These bones are not supposed to bear weight, and ulcers tend to develop beneath these pressure points. These ulcers can be a very complicated foot to manage, particularly when it is not recognized early.


You can read more about Charcot neuroarthropathy here, but the underlying idea is that a collapse of the arch can result in bones that normally don't bear weight becoming weight-bearing bones, and ulcers may develop in the mid arch or other odd locations.
10) We've mentioned shearing (friction) force as a cause of ulcers earlier. One common location for this is the edges of the heel. The most common reason for this would be a foot where the foot pronates significantly in gait, but this is exacerbated in open-heeled shoes (sandals, clogs), particularly when an autonomic neuropathy has altered the moisture balance in the skin.
Deep cracks and fissures (as seen below) can create perforate the skin, causing bleeding and infection.


11) Plantar heel ulcers (those on the bottom of the foot) are caused by forces that increase pressure on the heel. This can be caused by a “calcaneal gait,” a manner of ambulation where the posterior muscle group (back of the calf) is weakened, and the muscles on the front of the leg overpower those on the back. The ankle is bent forward in gait more than normal, keeping the weight on the heel for a greater portion of the gait cycle. Motor neuropathy alone may create this condition.
This is not a pattern of gait that is commonly recognized in the general medical community.
The condition may be affected by loss of the fat pad on the bottom of the foot and excess weight.
Plantar heel ulcers can be very difficult to treat because the key to healing ulcers is removing pressure, and people tend to put all their weight on their heels when they walk. Offloading through total contact casts, offloading boots and shoes will often resolve the wounds, though complete non-weightbearing may be required in some cases.




12) The opposite of a calcaneus gait is an equinus gait. In the equinus gait, it is the posterior (back of the calf) muscle group that overpowers the muscles on the front of the leg, causing the ankle to flex excessively, forcing the ball of the foot to bear too much weight.
Because the posterior muscle group is so much larger, equinus gait is much more common than a calcaneal gait. In fact, ulcers associated with equinus are so common that with every forefoot wound, equinus has to at least be considered as a possible factor.
Case report: The patient below had had recurrent ulcers across the midfoot for ten years. The photograph to the left was taken after 6 weeks of IV antibiotics, and the patient indicated this is as good as his feet have been in years. Perhaps, but those calluses are potential ulcer sites, and are a sign of danger
Equinus is the causative issue here, however, and a simple Tendo Achilles Lengthening performed under local anesthetic resolved the issue (below right).


13) We see the effect of too much force developing under one spot or another following amputations. For one example, when one or more metatarsals is amputated, the remaining metatarsals are forced to bear more weight, and ulcers in a new location are quite common, as seen below. We discuss this topic in greater detail on our page on amputation, but this is why amputations should be performed by someone with a very strong understanding of foot function.
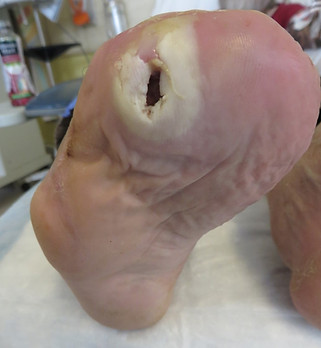
Biomechanics is a completely under-appreciated field of study in the development of ulcers, and ignoring biomechanical causes of ulcers is one of the reasons ulcers tend to recur at such a high rate.
Podiatrists (foot doctors) spend a great deal of time in understanding the mechanics of the foot, and this is one of several reasons they are so valuable in treating wounds. Statistics demonstrate the clear value of podiatrists treating wounds, as we discuss here.
To learn how pressure and shear damage the skin to create an ulcer, press here.
To return to the top of the page, click the maple leaf to the right
This page written by Dr. S A Schumacher
Podiatric Surgeon
Surrey, British Columbia Canada
Unless otherwise indicated, all clinical
photographs owned and provided by
Dr. S A Schumacher.
They may be reproduced for educational
purposes with attribution to:
Dr. S A Schumacher
