

Canadian
maple
Medical Alliance for the Preservation of the Lower Extremity
Achilles Tendon Lengthening
(When Your Achilles Tendon Is Your Achilles Heel)
Neuropathic ulcers are caused by a combination of two things:
-
Neuropathy (abnormal nerve function that can cause a variety of issues, including an inability to feel pain)
-
Pressure / Shear
The cause of that pressure can vary, depending on where the ulcer is located. For example, we discuss ulcers on the great toe and lesser toes on other pages.
But there are times when the excessive force is caused by a tight Achilles tendon that limits ankle motion.

The ankle normally has about 10 degrees of upward motion (dorsiflexion), as seen here.

However, some people have a limitation in ankle motion, as seen to the right. This foot has no dorsiflexion. Some patients can't even get to this position.
A lack of ankle joint motion is known as equinus, (pronounced
eh-kwy-nuss).
Without sufficient range of motion at the ankle, excessive pressure can develop in the ball of the foot as one walks.
In a non-diabetic, non-neuropathic patient, this can lead to metatarsalgia (pain in the ball of the foot), plantar fasciitis (strained arch), hammertoes, bunions and stiff great toe joints.

A tight Achilles can also cause calluses to form--often across multiple metatarsal bones, as seen to the right.
In neuropathic patients the pressure can result in blisters and ulcerations.
In this example you can see pressure is being exerted across the entire forefoot, as evidenced by multiple calluses. And there is an early blood blister forming (the dark discoloration) at the base of the 2nd toe.

In the neuropathic patient, this may progress to ulcerations--often across more than one metatarsal bone, as seen in these examples.






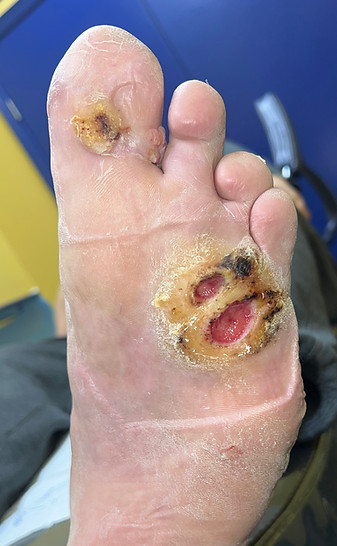
Ulcers under a single metatarsal can still have equinus as a factor in their formation.

But when one sees a single ulcer like the one to the right, it's important to first consider localized factors as a cause.

For example, when we look at the same ulcer from a different angle, we can see that the 1st metatarsal bone under the ulcer resides in a position lower the other metatarsals, and this is the cause of the extra pressure on this site and the cause of the ulcer formation.
In this case, an Achilles lengthening procedure would not address the cause of the ulcer and would not prove productive to resolving the ulcer.

To the right we see an example of another example of a localized cause for a metatarsal ulcer. In this case, the issue is an excessively long metatarsal.
Normally, the metatarsals form a parabolic shape, with the 2nd metatarsal longer than the 3rd, the 3rd longer than the 4th and the 4th longer than the 5th (yellow dashed lines).
However, here we see that the 3rd metatarsal (red arrow) is longer than the adjacent 2nd metatarsal. When walking, the foot rotates forward onto these bones, creating an unexpected point of pressure on the 3rd metatarsal, which may lead to an ulcer.
An Achilles tendon lengthening in this patient would be unlikely to resolve an ulcer here. Treatment for this ulcer would involve removal of pressure from this specific bone.
We have a separate page here to discuss metatarsal ulcerations and some of their causes and treatments at greater length.

Bony Equinus
In addition, not every case of equinus (limited ankle motion) is caused by a tight Achilles tendon.
Below we see an example of bony equinus, where there is limited ankle dorsiflexion, but it is not caused by a tight tendon. It is caused by arthritic changes at the front of the ankle joint, (white arrow).
This is best seen on a weight-bearing x-ray as a non-weight-bearing x-ray may allow the foot to plantarflex (ben down). The ankle may open up and it may not be as obvious that there is a bony bock present.
In this case, this bony equinus condition caused a forefoot ulcer, but a procedure to lengthen the tendon would not address the cause of the forefoot pressures causing the ulceration.

A high arched (or cavus) foot (below) can also be associated with limited ankle joint motion for mechanical reasons stemming from the front of the foot. These factors, too, need to be assessed before considering a Achilles lengthening procedure.

However, examples like these are less common than a tight Achilles tendon.
And while conservative care is still used to heal ulcers in cases involving the Achilles tendon, an Achilles tendon lengthening can be considered as a way to remove the causative force and potentially cure an ulcer.
The procedure may be appropriate in the following cases:
-
The ulcer is neuropathic in origin (i.e., not an ulcer caused by something else like poor blood flow)
-
The ulcer is on the bottom of the forefoot as seen in the examples here.
-
The ulcer is slow-to-heal with conservative care or the ulcer is recurrent.
-
There is limited ankle motion caused by a tight Achilles tendon and no other cause that might explain the ulcer.
How is the Achilles tendon lengthening performed?
The Achilles tendon (blue arrow) is the combined tendon from two muscles, the gastrocnemius (red arrow) and the soleus (black arrow).
The tendon can be lengthened through a variety of techniques. We'll discuss the two most common procedures. But first, let's look at the make up of the Achilles tendon.
The gastrocnemius muscle...
...and the soleus muscle...
...merge together near the ankle to form a common tendon--the Achilles tendon.

Note how the gastrocnemius muscle extends higher than the soleus and crosses the knee joint...
...whereas the soleus muscle
(seen here with the gastrocnemius removed from the diagram), does not extend as high, and does not cross the knee joint.

A Swedish physician named Nils Silfverskiöld noted that one could differentiate which Achilles fibers (gastrocnemius vs the combined gastrocnemius and soleus) were tight by performing a simple test we today call the Silfverskiöld test.

Nils Silfverskiöld
(1888-1957)
Nils Silfverskiöld also won a gold medal in gymnastics in the 1912 summer Olympics in Stockholm.
Silfverskiöld test
Because only the gastrocnemius muscle crosses the knee joint, Silfverskiöld realized that if the ankle was stiff when the knee was straight and the gastrocnemius was tight (below left), but exhibited more motion when the knee was bent and the gastrocnemius was relaxed, (below right), that the issue was a tight gastrocnemius.
In this case, only the gastrocnemius fibers needed to be released through a procedure known as a gastrocnemius recession.
If the ankle experienced limited motion regardless of whether the knee was straight, the combined tendon was tight and needed to be released. This is known as a Tendo Achilles Lengthening or TAL.


Causes of a Tight Achilles Tendon
The gastrocnemius (and not the soleus) becoming tightened is the more common issue. It can result from being sedentary and aging resulting in diminished flexibility. Overuse with specific activities like jumping, hill work, weights can also shorten the gastrocnemius, as can the use of high heel shoes.
Tightness involving both the gastrocnemius and soleus is less common. This can occur with immobilization (as with being placed in a cast) and neurological conditions (like stroke and cerebral palsy).
In diabetics, however, there can be another cause caused by high blood sugar--glycation. Glycation is where excessive sugar enters the collagen of the tendon making the tendon stiffer and less flexible.
Glycation
Glycation is an abnormal process where elevated blood sugars binds non-enzymatically to proteins such as collagen.
Glycation generally makes collagen stiffer, less elastic, and more brittle. It is associated with stiffening of the blood vessels, tendons, and joints. In the skin it contributes to wrinkling and visible aging of skin. It can also impair wound healing.
Glycation differs from glycosylation, which is a normal, enzyme-mediated process that adds sugars to protein or lipids, and is essential for normal tissue structure and function.
Tendo Achilles Lengthening Surgery and Gastroc Recession Surgery
In the gastrocnemius recession procedure, performed if only the gastrocnemius fibers are tight, a transverse cut (blue line) is made across the tendon just below the muscle belly of the gastrocnemius and above where the soleus fibers join the gastrocnemius tendon to form the Achilles tendon. This is performed through a small incision.
A common way to perform a Tendo Achilles Lengthening (if both the soleus and gastrocnemius fibers re tight) is by making three staggered cuts across the Achilles (green lines), with one cut located on one side of the tendon and two cuts on the other side. In gait, each cut will gap open a bit, effectively lengthening the tendon.
This is performed nearer to the heel bone where the two tendons (gastrocnemius and soleus) combine. It is performed with three small incisions.

Complications of Lengthening the Achilles Tendon
There are some potential complications with lengthening an Achilles tendon.
-
The major risk to this procedure is that sometimes the tendon is lengthened too much and a new ulcer forms at the heel (15%).
-
The tendon could rupture (4.3%) as the tendon is weaker from the procedure and, in diabetic patients, likely glycated (see above) from diabetes.
-
The patient can lose some strength in pushing off during gait. (Though, in the author's opinion, diminished push off power would be a fair trade for most patients compared to recurrent ulcerations.)
-
Though the incisions are quite small, they could be slow to heal or have a visible scar. (Though in the author's opinion, the risk of small incisions located away from the weight bearing surface is likely well below the risk of the ulcer on the bottom of the foot not healing.)
There are not a lot of studies comparing the recession with the TAL, but complications 1 and 2 would appear to be more likely when the entire tendon is lengthened and likely less common with the gastrocnemius recession procedure, where the soleus muscle and tendon are left intact.

Literature
According to a 2015 meta-analysis of 11 studies and 614 patients, both the gastrocnemius recession and the Tendo Achilles lengthening help diabetic plantar ulcers heal, at rates comparable to the gold standard, Total Contact Casting. Healing rates cited ranged from 86% to 100% in 57-76 days.
The biggest benefit of these procedures were the lower recurrence rate--which was 55% lower than the Total Contact Cast. Complications were 15% developed a heel ulcer, 6.5% a hematoma and 4.3% an Achilles rupture.
Dallimore SM, Kaminski MR. Tendon lengthening and fascia release for healing and preventing diabetic foot ulcers: a systematic review and meta-analysis. J Foot Ankle Res. 2015;8:33.
Our Bottom Line:
The procedure is not without risks, but in the right cases, (forefoot ulcers that are struggling to heal or recurrent)...
Surgically lengthening the Achilles tendon can be as effective as Total Contact Casts at healing a wound
and it can cut the re-ulceration rate in half.
Before and After




To return to the top of this page, click on the leaf to the right.
This page written by Dr. S A Schumacher
Podiatric Surgeon
Surrey, British Columbia Canada
Unless otherwise indicated, all clinical
photographs owned and provided by
Dr. S A Schumacher.
They may be reproduced for educational
purposes with attribution to:
Dr. S A Schumacher
